A new study reveals that the SARS-CoV-2 virus infects cells by binding a single virus to a single ACE2 receptor, contrary to previous theories. This was discovered through super-resolution microscopy which also showed a low density of ACE2 receptors on cell membranes, challenging the possibility of a virus particle binding to multiple receptors simultaneously. This new understanding could help in devising improved COVID-19 prevention and treatment methods.
In Europe, the pandemic triggered in 2020 by the SARS-CoV-2 coronavirus is now largely under control. But why this virus is able to spread so efficiently remains unclear. A team of researchers led by Dr. Simone Backes, Dr. Gerti Beliu, and Prof. Dr. Markus Sauer of the Julius Maximilian University of Würzburg (JMU) has now shown in a publication in Angewandte Chemie that some previous assumptions need to be reconsidered.
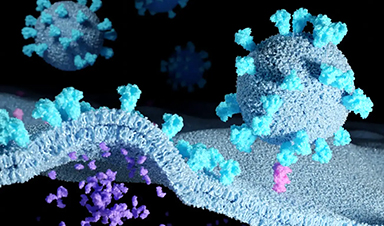
For example, the virus does not bind with several surface proteins simultaneously to several receptors of the cell to be infected. This assumption has previously been an attempt to explain how viruses increase their infectivity. Binding to a single receptor also does not lead to the subsequent docking of further receptors to the virus. The Würzburg research group has now provided evidence that a single virus binds to a single receptor, opening the door for a highly efficient infection.
What could only be speculated about
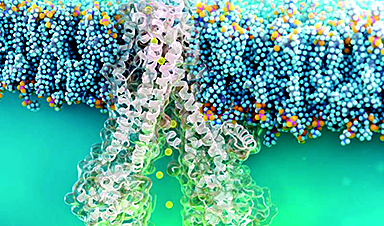
SARS-CoV-2 carries an average of 20 – 40 spike proteins on its surface. With these, it binds to ACE2 receptors in the membrane of its target cells, for example in the nose and throat of humans. When these receptors are blocked with antibodies, the cell can no longer be infected. "This suggests that the binding of the virus to the ACE2 receptor is the decisive step in infection," Sauer explains.
Making the ACE2 receptors and their interaction with the viral spike proteins visible microscopically has not been possible so far. Therefore, much was left to speculation — such as whether the viruses bind to multiple receptors with multiple spikes to facilitate entry into the cell.
It was also considered that the receptors are present in the membrane in pairs or groups of three rather, so that they can bind more efficiently to the trimeric spike proteins. Or that they are only combined into such groups after binding to a spike protein. Both depend strongly on the density of the ACE2 receptors in the membrane.
Super-resolution microscopy made it clear
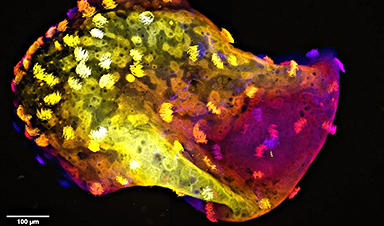
The Würzburg researchers wanted to elucidate this mystery: They labeled antibodies with dyes to make the receptors visible and countable. To do this, they used various cell lines that are used as model systems for SARS-CoV infection, and the single-molecule sensitive super-resolution microscopy method dSTORM, developed in Markus Sauer's research group.
It turned out that Vero cells, for example, which are often used as a model for SARS-CoV-2 infection, only have one to two ACE2 receptors per square micrometer of cell membrane. This is very few: "In other membrane receptors, this number is often between 30 and 80," Sauer added.
"The average distance between neighboring ACE2 receptors is about 500 nanometers. It is thus much larger than a virus particle, which measures only 100 nanometres," says Backes. The idea that a virus particle with multiple spike proteins can bind to multiple receptors simultaneously is therefore very unlikely, she adds.
ACE2 receptors are always single
The following open question: Are the receptors also present as pairs or groups of three in the membrane? "No. They only occur there singly. And it stays that way even when a viral spike protein has bound to them," says Beliu, group leader at the Rudolf Virchow Centre. For an infection, it is sufficient if a single spike binds to a single receptor.
With these results, the JMU team was able to disprove many of the original hypotheses about the interaction of viral particles with multiple ACE2 receptors. It also showed that host cells with higher ACE2 expression are more easily infected, as expected. However, the lipid composition of the membrane and other factors also influence infection efficiency.
What is next?
The JMU team wants to gather as much detailed knowledge as possible about the cell entry mechanism of coronaviruses in order to better understand the infection process. This could ultimately contribute to better prevention and the development of better drugs against COVID-19. Next, the Würzburg researchers want to analyze the entry mechanism with high-resolution light sheet microscopy.
Reference: "Coronaviruses Use ACE2 Monomers as Entry-Receptors" by Dr. Patrick Eiring, Dr. Teresa Klein, Dr. Simone Backes, Marcel Streit, Marvin Jungblut, Dr. Sören Doose, Dr. Gerti Beliu and Prof. Dr. Markus Sauer, 27 March 2023, Angewandte Chemie.
DOI: 10.1002/anie.202300821
The work described was funded by the European Research Council, the German Research Foundation, and the German Federal Ministry of Education and Research.
News
Bowel and Ovarian Cancers Are Dramatically Rising in Young Adults, Scientists Aren’t Sure Why
Cancer incidence is increasing, especially among younger adults, and current risk factors don’t fully account for the trend. Scientists suggest other underlying causes may be contributing. Cancer patterns in England are shifting in a [...]
New Immune Pathway Could Supercharge mRNA Cancer Vaccines
A surprising backup system in the immune response to mRNA vaccines may hold the key to more effective cancer treatments. The arrival of mRNA vaccines against SARS-CoV-2 in 2020 marked a turning point in the COVID-19 pandemic. Today, [...]
Scientists Discover “Molecular Switch” That Fuels Alzheimer’s Brain Inflammation
A newly identified trigger of brain inflammation could offer a fresh target for slowing Alzheimer’s progression. The brain has its own built-in immune system that identifies threats and responds to them. In Alzheimer’s disease, growing evidence [...]
Molecular Manufacturing: The Future of Nanomedicine – New book from NanoappsMedical Inc.
This book explores the revolutionary potential of atomically precise manufacturing technologies to transform global healthcare, as well as practically every other sector across society. This forward-thinking volume examines how envisaged Factory@Home systems might enable the cost-effective [...]
Forgotten Medicinal Plant Shows Promise in Fighting Dangerous Superbugs
A traditional medicinal plant, tormentil, shows promise against antibiotic-resistant bacteria in laboratory tests. Its compounds work by limiting bacterial growth and boosting antibiotic performance. Before the development of modern antibiotics, plant-based remedies were commonly [...]
NanoMedical Brain/Cloud Interface – Explorations and Implications. A new book from Frank Boehm
New book from Frank Boehm, NanoappsMedical Inc Founder: This book explores the future hypothetical possibility that the cerebral cortex of the human brain might be seamlessly, safely, and securely connected with the Cloud via [...]
New Research Finds Shocking Link Between Chili Peppers and Cancer
If you love spicy food, you are not alone. But scientists are taking a closer look at whether eating a lot of chili peppers could affect your cancer risk. Could your love of spicy [...]
New book from Nanoappsmedical Inc. – Global Health Care Equivalency
A new book by Frank Boehm, NanoappsMedical Inc. Founder. This groundbreaking volume explores the vision of a Global Health Care Equivalency (GHCE) system powered by artificial intelligence and quantum computing technologies, operating on secure [...]
Scientists Create “Neurobots” – Living Machines With Their Own Nervous Systems
Neurobots—xenobots with neurons—show self-organized nervous systems and enhanced behaviors, revealing new insights into how biology builds functional structures. In 2020, researchers at Tufts University developed tiny living structures known as xenobots using frog cells. These microscopic organisms [...]
Our books now available worldwide!
Online Sellers other than Amazon, Routledge, and IOPP Indigo Global Health Care Equivalency in the Age of Nanotechnology, Nanomedicine and Artifcial Intelligence Global Health Care Equivalency In The Age Of Nanotechnology, Nanomedicine And Artificial [...]
Amazonian Chocolate Could Become the Next Superfood, Scientists Say
New research into Amazonian cocoa reveals that its value may extend beyond flavor alone. Chocolate from the Amazon is already known worldwide for its distinctive taste, but new research suggests it may offer even [...]
Nanobody repairs misfolded CFTR inside cells, boosting function in cystic fibrosis
A tiny antibody component could fundamentally transform the treatment of cystic fibrosis: For the first time, researchers have succeeded in developing a so-called nanobody that penetrates directly into human cells and can repair the [...]
20-Year Study Finds Daily Multivitamins Don’t Extend Lifespan
A large, decades-long study of over 390,000 U.S. adults challenges a widespread assumption about daily multivitamins. Multivitamins are a daily habit for millions of Americans, often taken with the expectation that they will extend [...]
Novel Investment Paradigms for Regenerative Healthcare Ecosystems
Introduction The transition toward regenerative healthcare ecosystems—anchored in wellness optimization, disease prevention, eradication strategies, and healthy longevity—necessitates a structural reconfiguration of capital architectures, governance models, and incentive design. Regenerative healthcare, by definition, transcends episodic [...]
What If Consciousness Exists Beyond Your Brain
Scientists still don’t know how consciousness emerges from the brain. New ideas suggest it may not emerge at all, but instead be a basic feature of reality. Is consciousness produced by the brain, or [...]
Scientists Discover Way To Treat Lung Cancer and Its Deadly Side Effect Together
A new approach using lipid nanoparticles to deliver genetic material is showing promise in tackling two major challenges in lung cancer at once.Researchers at Oregon State University have designed a new way to tackle two of [...]