Recent research reveals a breakthrough in lung repair, showing how delivering VEGFA via lipid nanoparticles can significantly repair damaged blood vessels, akin to plumbing repairs. This method, validated in animal models, offers promising insights into treating respiratory virus damages, enhancing oxygen delivery, and reducing lung inflammation and scarring.
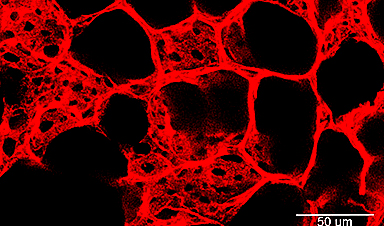
In the human body, the lungs and their vasculature can be likened to a building with an intricate plumbing system. The lungs' blood vessels are the pipes essential for transporting blood and nutrients for oxygen delivery and carbon dioxide removal. Much like how pipes can get rusty or clogged, disrupting normal water flow, damage from respiratory viruses, like SARS-CoV-2 or influenza, can interfere with this "plumbing system."
In a recent study, researchers looked at the critical role of vascular endothelial cells in lung repair. Their work, published in Science Translational Medicine, was led by Andrew Vaughan of the University of Pennsylvania's School of Veterinary Medicine and shows that, by using techniques that deliver vascular endothelial growth factor alpha (VEGFA) via lipid nanoparticles (LNPs), that they were able to greatly enhance modes of repair for these damaged blood vessels, much like how plumbers patch sections of broken pipes and add new ones.
Advanced Research Findings
"While our lab and others have previously shown that endothelial cells are among the unsung heroes in repairing the lungs after viral infections like the flu, this tells us more about the story and sheds light on the molecular mechanisms at play," says Vaughan, assistant professor of biomedical sciences at Penn Vet. "Here we've identified and isolated pathways involved in repairing this tissue, delivered mRNA to endothelial cells, and consequently observed enhanced recovery of the damaged tissue. These findings hint at a more efficient way to promote lung recovery after diseases like COVID-19."
They found VEGFA's involvement in this recovery, while building on work in which they used single cell RNA sequencing to identify transforming growth factor beta receptor 2 (TGFBR2) as a major signaling pathway. The researchers saw that when TGFBR2 was missing it stopped the activation of VEGFA. This lack of signal made the blood vessel cells less able to multiply and renew themselves, which is vital for the exchange of oxygen and carbon dioxide in the tiny air sacs of the lungs.
"We'd known there was a link between these two pathways, but this motivated us to see if delivering VEGFA mRNA into endothelial cells could improve lung recovery after disease-related injury," says first author Gan Zhao, a postdoctoral researcher in the Vaughan Lab.
Innovative Delivery Methods
The Vaughan Lab then reached out to Michael Mitchell of the School of Engineering and Applied Science, whose lab specializes in LNPs, to see if delivery of this mRNA cargo would be feasible.
"LNPs have been great for vaccine delivery and have proven incredibly effective delivery vehicles for genetic information. But the challenge here was to get the LNPs into the bloodstream without them heading to the liver, which is where they tend to congregate as its porous structure lends favor to substances passing from the blood into hepatic cells for filtration," says Mitchell, an associate professor of bioengineering at Penn Engineering and a coauthor of the paper. "So, we had to devise a way to specifically target the endothelial cells in the lungs."
Lulu Xue, a postdoctoral researcher in the Mitchell Lab and a co-first author of the paper, explains that they engineered the LNP to have an affinity for lung endothelial cells, this is known as extra hepatic delivery, going beyond the liver.
"We've seen evidence in the literature suggesting it's doable, but the systems we'd seen are made up of positively charged lipids which were too toxic," Xue says. "This led me to developing an ionizable lipid that's not positively charged when it enters the bloodstream but gets charged when it gets to the endothelial cells, thereby releasing the mRNA."
Their LNPs proved effective in delivering VEGFA into endothelial cells and as a result, the researchers saw a marked improvement in vascular recovery in their animal models. Within the animal models, the researchers saw improved oxygen levels, and in some, the treatment helped them recover their weight better than the control group. These treated mice also had less lung inflammation, shown by lower levels of certain markers in their lung fluid, and their lungs showed less damage and scarring, with more healthy blood vessels.
"Although we went in hoping for this outcome, it was a real thrill to see how effective, safe, and efficiently this all panned out, so we're looking forward to testing this delivery platform for other cell types in the lung, and it will be important to evaluate whether TGFB signaling is important in other injury contexts including chronic conditions like emphysema and COPD," Vaughan says. "With this proof-of-concept being well validated, we're sure that we'll pave the way for new mRNA-based strategies for treating lung injury."
Reference: "TGF-βR2 signaling coordinates pulmonary vascular repair after viral injury in mice and human tissue" by Gan Zhao, Lulu Xue, Aaron I. Weiner, Ningqiang Gong, Stephanie Adams-Tzivelekidis, Joanna Wong, Maria E. Gentile, Ana N. Nottingham, Maria C. Basil, Susan M. Lin, Terren K. Niethamer, Joshua M. Diamond, Christian A. Bermudez, Edward Cantu, Xuexiang Han, Yaqi Cao, Mohamad-Gabriel Alameh, Drew Weissman, Edward E. Morrisey, Michael J. Mitchell and Andrew E. Vaughan, 31 January 2024, Science Translational Medicine.
DOI: 10.1126/scitranslmed.adg6229
Andrew Vaughan is an assistant professor in the Department of Biomedical Sciences at the University of Pennsylvania School of Veterinary Medicine.
Michael Mitchell is an associate professor in the Department of Bioengineering in the School of Engineering and Applied Science and the director of the Lipid Nanoparticle Synthesis Core at the Penn Institute for RNA Innovation at the University of Pennsylvania.
Gan Zhao is a postdoctoral researcher in the Vaughn Lab at Penn Vet.
Lulu Xue is a postdoctoral researcher in the Mitchell Lab at Penn Engineering.
Other authors include Stephanie Adams-Tzivelekidis, Maria E. Gentile, Aaron I. Weiner, and Joanna Wong from Penn Vet; Ningqiang Gong and Xuexiang Han from Penn Engineering; and Mohamad-Gabriel Alameh, Maria C. Basil, Christian A. Bermudez, Edward Cantu, Yaqi Cao, Joshua M. Diamond, Susan M. Lin, Edward E. Morrisey, Terren K. Niethamer, Ana N. Nottingham, and Drew Weissman in the Perelman School of Medicine at Penn.
This work was supported by the National Institutes of Health (grants R01HL153539 and R01HL164350 and award DP2 TR002776, the Margaret Q. Landenberger Foundation, a Burroughs Wellcome Fund Career Award at the Scientific Interface; and the National Science Foundation (Award CBET-2145491).
News
Scientists Just Found a Surprising Way To Destroy “Forever Chemicals”
Scientists have uncovered a new mechanism that may help break down highly persistent PFAS pollutants. PFAS have earned the nickname “forever chemicals” for a reason. These industrial compounds are so chemically durable that they [...]
Scientists Discover Cheap Material That Kills Deadly Superbugs
A new sulfur-rich antimicrobial polymer shows strong effectiveness against fungal and bacterial pathogens and may offer an affordable solution to antimicrobial resistance. Antimicrobial resistance is creating growing challenges for both healthcare and food production, [...]
What to Know About Cicada, or BA.3.2, the Latest SARS-CoV-2 Variant Under Monitoring
Like periodical cicadas, the insects for which it is nicknamed, SARS-CoV-2 Omicron subvariant BA.3.2 is only just beginning to emerge after lying low for an extended period since it first appeared. Although it was [...]
Scientists Say This Simple Supplement May Actually Reverse Heart Disease
Scientists in Japan say a common supplement may actually help “unclog” certain diseased heart arteries from the inside out. A simple food supplement sold in Japan may have helped reverse a dangerous form of [...]
New breakthrough against radiation: Korean Scientists create revolutionary shield with nanotechnology
Korean Scientists develop new nanotechnology material capable of reducing radiation impacts in space missions, hospitals, and power plants. The search for more efficient protection technologies in extreme environments has just gained an important advance. Korean [...]
Scientists Just Discovered the Hidden Trick That Keeps Your Cells Alive
A strange bead-like motion inside cells may be the secret to keeping their DNA—and health—in balance. Mitochondria are often described as the power plants of the cell because they produce the energy cells need [...]
Scientists Discover Stem Cells That Could Regrow Teeth and Bone
Scientists just uncovered the cellular “blueprint” that could one day let us regrow real teeth. Researchers at Science Tokyo have uncovered two distinct stem cell lineages that play a central role in forming tooth [...]
Scientists Uncover Fatal Weakness in “Zombie Cells” Linked to Cancer
A newly identified weakness in “zombie” cells may open the door to more precise cancer treatments by turning their own survival strategy against them. A new class of drugs takes advantage of a recently [...]
Bowel and Ovarian Cancers Are Dramatically Rising in Young Adults, Scientists Aren’t Sure Why
Cancer incidence is increasing, especially among younger adults, and current risk factors don’t fully account for the trend. Scientists suggest other underlying causes may be contributing. Cancer patterns in England are shifting in a [...]
New Immune Pathway Could Supercharge mRNA Cancer Vaccines
A surprising backup system in the immune response to mRNA vaccines may hold the key to more effective cancer treatments. The arrival of mRNA vaccines against SARS-CoV-2 in 2020 marked a turning point in the COVID-19 pandemic. Today, [...]
Scientists Discover “Molecular Switch” That Fuels Alzheimer’s Brain Inflammation
A newly identified trigger of brain inflammation could offer a fresh target for slowing Alzheimer’s progression. The brain has its own built-in immune system that identifies threats and responds to them. In Alzheimer’s disease, growing evidence [...]
Molecular Manufacturing: The Future of Nanomedicine – New book from NanoappsMedical Inc.
This book explores the revolutionary potential of atomically precise manufacturing technologies to transform global healthcare, as well as practically every other sector across society. This forward-thinking volume examines how envisaged Factory@Home systems might enable the cost-effective [...]
Forgotten Medicinal Plant Shows Promise in Fighting Dangerous Superbugs
A traditional medicinal plant, tormentil, shows promise against antibiotic-resistant bacteria in laboratory tests. Its compounds work by limiting bacterial growth and boosting antibiotic performance. Before the development of modern antibiotics, plant-based remedies were commonly [...]
NanoMedical Brain/Cloud Interface – Explorations and Implications. A new book from Frank Boehm
New book from Frank Boehm, NanoappsMedical Inc Founder: This book explores the future hypothetical possibility that the cerebral cortex of the human brain might be seamlessly, safely, and securely connected with the Cloud via [...]
New Research Finds Shocking Link Between Chili Peppers and Cancer
If you love spicy food, you are not alone. But scientists are taking a closer look at whether eating a lot of chili peppers could affect your cancer risk. Could your love of spicy [...]
New book from Nanoappsmedical Inc. – Global Health Care Equivalency
A new book by Frank Boehm, NanoappsMedical Inc. Founder. This groundbreaking volume explores the vision of a Global Health Care Equivalency (GHCE) system powered by artificial intelligence and quantum computing technologies, operating on secure [...]