Antimicrobial resistance poses a significant threat to humanity, health leaders have warned, as a study reveals it has become a leading cause of death worldwide and is killing about 3,500 people every day.
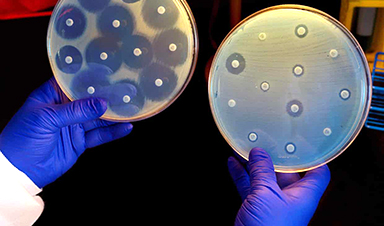
More than 1.2 million – and potentially millions more – died in 2019 as a direct result of antibiotic-resistant bacterial infections, according to the most comprehensive estimate to date of the global impact of antimicrobial resistance (AMR).
The stark analysis covering more than 200 countries and territories was published in the Lancet. It says AMR is killing more people than HIV/Aids or malaria. Many hundreds of thousands of deaths are occurring due to common, previously treatable infections, the study says, because bacteria that cause them have become resistant to treatment.
“We need to leverage this data to course-correct action and drive innovation if we want to stay ahead in the race against antimicrobial resistance.”
Previous estimates of the health impact of AMR have been published for several countries and regions, and for a small number of pathogen-drug combinations in a wider range of locations. However, until now no estimates have covered all locations or a broad range of pathogens and drug combinations.
The new Global Research on Antimicrobial Resistance (Gram) report estimates deaths linked to 23 pathogens and 88 pathogen-drug combinations across 204 countries and territories in 2019. Statistical modelling was used to produce estimates of the impact of AMR in all locations – including those with no data – using more than 470m individual records obtained from systematic literature reviews, hospital systems, surveillance systems, and other data sources.
The analysis shows AMR was directly responsible for an estimated 1.27million deaths worldwide, and associated with an estimated 4.95 million deaths, in 2019. HIV/Aids and malaria have been estimated to have caused 860,000 and 640,000 deaths, respectively, in 2019.
While AMR poses a threat to people of all ages, young children were found to be at particularly high risk, with one in five deaths attributable to AMR occurring in children under the age of five.
The report highlights an urgent need to scale up action to combat AMR, and outlines immediate actions for policymakers that would help save lives and protect health systems. These include optimising the use of existing antibiotics, taking greater action to monitor and control infections, and providing more funding to develop new antibiotics and treatments.
The UK’s special envoy on antimicrobial resistance, Dame Sally Davies, said AMR was “one of the greatest challenges facing humanity”. She added: “Behind these new numbers are families and communities who are tragically bearing the brunt of the silent AMR pandemic. We must use this data as a warning signal to spur on action at every level.”
Regionally, deaths caused directly by AMR were estimated to be highest in sub-Saharan Africa and south Asia, at 24 deaths per 100,000 population and 22 deaths per 100,000 population respectively.
In high-income countries, AMR led directly to 13 deaths per 100,000 and was associated with 56 deaths per 100,000. In the western Europe region, which includes the UK, more than 51,000 people died as a direct result of AMR.
Other experts said Covid-19 had demonstrated the importance of global commitments to infection and control measures, such as hand-washing and surveillance, and rapid investments in treatments.
Tim Jinks, the head of the drug-resistant infections programme at Wellcome Trust, said: “The Covid-19 pandemic has highlighted the importance of global collaboration: political leaders, the healthcare community, the private sector and the public working together to tackle a global health threat.
“Like Covid-19, we know what needs to be done to address AMR, but we must now come together with a sense of urgency and global solidarity if we are to be successful.”