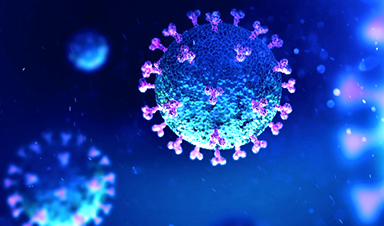
The hubbub around mutations in the virus that causes COVID-19—and how they might make it more infectious—has been around since the early phase of the pandemic. A preprint study about a particular mutation involving the “spikes” studding the SARS-CoV-2 pathogen had previously drawn attention, and that investigation has now been peer-reviewed and published in Cell. The paper details a change in one amino acid in the virus that may have made it more infectious. But virologists are far from a consensus about the possible role of this mutation.
The paper indicates that a single amino acid change from D (aspartic acid) to G (glycine) on the SARS-CoV-2 spike protein (which such viruses use to grab onto human cells) is the key to how infectious the pathogen is. “The spike protein has a critically important role in the biology of the virus,” says Bette Korber, a computational biologist at the Los Alamos National Laboratory and lead author of the new paper.
Korber and her colleagues came to this conclusion after employing multiple approaches to examine the two strains. First, they performed a statistical analysis that showed how the mutated virus—often referred to as the “G strain”—achieved dominance across multiple continents, outperforming the coexisting original version of SARS-CoV-2, or “D strain.” Then the researchers tested the amount of the virus in individuals with COVID-19 at the Sheffield Teaching Hospitals NHS Foundation Trust in England. The results showed that the G strain produced more of the virus in the human body than the D strain. But the former did not lead to a higher hospitalization rate, meaning it apparently did not cause more severe illnesses. Lastly, the team members created “pseudotype” pathogens by embedding SARS-CoV-2 spike proteins, containing either D or G amino acids, into other disease-causing viruses. They tested these pseudotype viruses by infecting human cells in a lab dish, and the result suggested that the G-bearing one was more infectious. Examining cells in a dish, however, is not the same as testing them using “multiple cell types with an immune system in a human body,” says Emma Hodcroft, a molecular epidemiologist at the University of Basel in Switzerland, who was not involved in the study. “We just have to be really careful with how far we take the conclusions.”
Image Credit: Amanda Scott/ Alias
![]()
News This Week
Simple Fiber Supplement Cuts Knee Arthritis Pain in Just 6 Weeks, Study Finds
A daily inulin supplement may help reduce knee osteoarthritis pain while revealing a possible link between gut health, muscle function, and pain sensitivity. For millions of people living with knee osteoarthritis, managing chronic pain [...]
This Common Vitamin May Help Stop Prediabetes From Turning Into Diabetes
Vitamin D may help prevent type 2 diabetes in people with specific genetic variations, offering a possible path toward personalized diabetes prevention. More than 40% of U.S. adults have prediabetes, a condition in which [...]
Ebola, hantavirus: Is the world prepared for the next pandemic?
Funding cuts to health research and a growing antivaccine movement are making it harder than ever to respond to viruses. The World Health Organization (WHO) has declared that an Ebola outbreak in Uganda and [...]
May 2026 Healthcare News and Trends: Market Signals That Matter
Artificial intelligence is dominating headlines, telehealth has settled into a new normal, and digital health continues to promise transformation. However, much of what is being discussed in healthcare today reflects potential rather than reality. [...]
Scientists Rewire Donor Stem Cells To Outsmart Aggressive Blood Cancers
Researchers have tested a gene-edited stem cell transplant designed to shield healthy blood-forming cells from powerful cancer-targeting immunotherapies. For patients with highly aggressive blood cancers, stem cell transplantation can offer a rare chance at [...]
Recent Digital Health Trends, Insights and News – May 2026
Last month marked continued progress as digital health moves into its next phase — from AI expanding into drug discovery and core infrastructure to new federal pathways accelerating device access and home-based care. Together, [...]
Cancer Mystery Solved: Scientists Discover How Melanoma Becomes “Immortal”
Scientists have uncovered a previously overlooked mechanism that may help melanoma cells become effectively “immortal.” Cancer cells face a major problem before they can become deadly: They have to figure out how to stop [...]
How Visual Neurons Organize Thousands of Synaptic Inputs
Summary: A new study uncovered the organizational rules that determine how neurons in the primary visual cortex process information. By imaging both the cell bodies (soma) and the individual synapses (on dendritic spines) of [...]
Scientists Just Found a Surprising Way To Destroy “Forever Chemicals”
Scientists have uncovered a new mechanism that may help break down highly persistent PFAS pollutants. PFAS have earned the nickname “forever chemicals” for a reason. These industrial compounds are so chemically durable that they [...]
Scientists Discover Cheap Material That Kills Deadly Superbugs
A new sulfur-rich antimicrobial polymer shows strong effectiveness against fungal and bacterial pathogens and may offer an affordable solution to antimicrobial resistance. Antimicrobial resistance is creating growing challenges for both healthcare and food production, [...]
What to Know About Cicada, or BA.3.2, the Latest SARS-CoV-2 Variant Under Monitoring
Like periodical cicadas, the insects for which it is nicknamed, SARS-CoV-2 Omicron subvariant BA.3.2 is only just beginning to emerge after lying low for an extended period since it first appeared. Although it was [...]
Scientists Say This Simple Supplement May Actually Reverse Heart Disease
Scientists in Japan say a common supplement may actually help “unclog” certain diseased heart arteries from the inside out. A simple food supplement sold in Japan may have helped reverse a dangerous form of [...]
New breakthrough against radiation: Korean Scientists create revolutionary shield with nanotechnology
Korean Scientists develop new nanotechnology material capable of reducing radiation impacts in space missions, hospitals, and power plants. The search for more efficient protection technologies in extreme environments has just gained an important advance. Korean [...]
Scientists Just Discovered the Hidden Trick That Keeps Your Cells Alive
A strange bead-like motion inside cells may be the secret to keeping their DNA—and health—in balance. Mitochondria are often described as the power plants of the cell because they produce the energy cells need [...]
Scientists Discover Stem Cells That Could Regrow Teeth and Bone
Scientists just uncovered the cellular “blueprint” that could one day let us regrow real teeth. Researchers at Science Tokyo have uncovered two distinct stem cell lineages that play a central role in forming tooth [...]
Scientists Uncover Fatal Weakness in “Zombie Cells” Linked to Cancer
A newly identified weakness in “zombie” cells may open the door to more precise cancer treatments by turning their own survival strategy against them. A new class of drugs takes advantage of a recently [...]