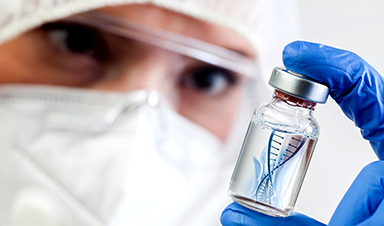
“It is a very serious disease with serious complications from which patients die relatively young,” says hematologist Linet Njue, senior physician at Inselspital Bern. According to the doctor, around 100 patients with the disease are being treated in large university hospitals in Switzerland, but the exact number is not recorded. It is one of the most common hereditary diseases worldwide.
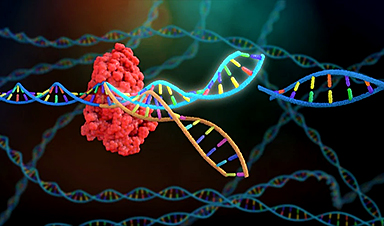
The disease is caused by a gene that carries the blueprint for the red blood pigment haemoglobin. A gene mutation crystallizes the hemoglobin, causing the normally round red blood cells to deform into sickles. These, in turn, clog the bloodstream.
Now, the UK Medicines Agency has given the green light for a new gene therapy for sickle cell anaemia patients aged 12 and over. It is called Exacel (brand name “Casgevy”) and was developed by the companies Vertex Pharmaceuticals and CRISPR Therapeutics, the latter based in Zug.
It is the first ever approved treatment based on the CRISPR/Cas9 gene scissors. This is the technology that can precisely cut through and modify the genetic material and for the discovery of which the Nobel Prize in Chemistry was awarded in 2020.
No need for a foreign donor anymore
Victoria Gray, now 37, was the first person to be treated with the therapy in 2019. Thanks to the new “supercells”, her life has changed completely, she recently said. She now lives free of pain, can go back to work and take care of her four children.
Exacel has now been tested on around forty sickle cell anemia patients. As Vertex Pharmaceuticals and CRISPR Therapeutics have announced, additional clinical trials with children between the ages of 2 and 11 are now to begin. An application for approval for the therapy has not yet been received from the companies in Switzerland, as Swissmedic confirmed on request.
How Exacel Therapy WorksExacel does not target the disease-causing and mutated HBB gene, which causes the sickle-shaped blood cells. Rather, the therapy is dedicated to the gene called BCL11A. This gene is activated at birth and thus inhibits the formation of haemoglobin, which is actually only produced in the fetus. Exacel then cuts BCL11A apart, which deactivates the gene again and resumes prenatal hemoglobin production. This provides additional hemoglobin that is not malformed. The symptoms of the disease disappear. (sny)
Jacob Corn is Professor of Genome Biology at ETH Zurich and has been working on CRISPR treatments for years, including for sickle cell disease. “The whole CRISPR community is in a frenzy. The Exacel successes are impressive,” he says.
Nevertheless, it is crucial to accompany the treated patients over a long period of time, the regulatory authorities require at least 15 years. This is the only way to rule out long-term side effects, such as an increased risk of blood cancer – a concern that worries some scientists. However, Corn emphasizes: “At the moment, things are looking really good.”
According to the ETH professor, the CRISPR gene scissors offer a gateway to a new world of medicine. He draws a comparison:
It’s the same with hereditary diseases so far: You can make a genetic diagnosis to suffering patients, but you can’t offer them a therapy – that’s changing now.
There are more than 7000,1 diseases that are based on a single gene mutation, such as sickle cell anemia, and dozens of therapies are already in the pipeline, for example against the metabolic disease called familial hypercholesterolemia, which affects about 200 in <> people in Switzerland.
Due to the disease, a dangerous amount of cholesterol always remains in the blood. This greatly increases the risk of a heart attack or stroke. Studies with the CRISPR therapy from the biotech company Verve Therapeutics have so far been promising, even suggesting that “the world’s biggest killer” can soon be stopped, according to the headline of the US magazine “MIT Technology Review”.
Targeting multiple genes is much more difficult
Other diseases in the focus of the genetic engineers are cystic fibrosis, Duchenne muscular dystrophy or progeria, in which affected children age as if in fast motion. In addition to these single-mutation diseases, there are countless other diseases that are based on a combination of several gene mutations and environmental factors: Alzheimer’s, arthritis, many cancers, diabetes, autism spectrum disorders are just a few examples.
Another hurdle of future CRISPR therapies is those diseases that affect organs that are difficult to reach. In sickle cell anemia, it is comparatively easy to extract the blood cells from the body, manipulate them and return them. “In cystic fibrosis, on the other hand, where the lungs are damaged, it is a much more difficult procedure to get the genetic medicine to the right place,” says Corn.
The high cost could limit availability
Geneticists are very worried about the horrendous costs, which are estimated to run into the millions for a single CRISPR treatment. It is questionable whether poorer countries can afford such therapies. Even rich countries get into trouble when a large number of patients suddenly want to be treated.
One dilemma, according to Jacob Corn, is that the safety requirements imposed by the health authorities are enormously high – and therefore costly. “That’s good, because it must be guaranteed that the therapies do no more harm than good.” The hope is that after the first approvals, the multitude of safety and efficacy tests will no longer have to be carried out every single time. “If the safety of CRISPR technology is proven on its own, then hopefully it would be legitimate to accelerate the testing and approval of therapies for other diseases,” says Corn.
Another approach: Instead of isolating the cells for the gene changes, treating them and then injecting them back into the body, researchers are tinkering with a gene injection: “The idea is that the genome editing process is injected into the body, so to speak, where it finds the right place and exerts its effect.” This would not only make treatment cheaper, but also more accessible, for example in regions of Africa where there are few health facilities. No tests have yet been carried out in humans, only in animals.
But Jacob Corn is confident: “A large number of research groups around the world are involved in CRISPR. How quickly things can sometimes happen when many bright minds are working on a problem at the same time was seen with the Corona vaccination.” (aargauerzeitung.ch)
News
Cancer Mystery Solved: Scientists Discover How Melanoma Becomes “Immortal”
Scientists have uncovered a previously overlooked mechanism that may help melanoma cells become effectively “immortal.” Cancer cells face a major problem before they can become deadly: They have to figure out how to stop [...]
How Visual Neurons Organize Thousands of Synaptic Inputs
Summary: A new study uncovered the organizational rules that determine how neurons in the primary visual cortex process information. By imaging both the cell bodies (soma) and the individual synapses (on dendritic spines) of [...]
Scientists Just Found a Surprising Way To Destroy “Forever Chemicals”
Scientists have uncovered a new mechanism that may help break down highly persistent PFAS pollutants. PFAS have earned the nickname “forever chemicals” for a reason. These industrial compounds are so chemically durable that they [...]
Scientists Discover Cheap Material That Kills Deadly Superbugs
A new sulfur-rich antimicrobial polymer shows strong effectiveness against fungal and bacterial pathogens and may offer an affordable solution to antimicrobial resistance. Antimicrobial resistance is creating growing challenges for both healthcare and food production, [...]
What to Know About Cicada, or BA.3.2, the Latest SARS-CoV-2 Variant Under Monitoring
Like periodical cicadas, the insects for which it is nicknamed, SARS-CoV-2 Omicron subvariant BA.3.2 is only just beginning to emerge after lying low for an extended period since it first appeared. Although it was [...]
Scientists Say This Simple Supplement May Actually Reverse Heart Disease
Scientists in Japan say a common supplement may actually help “unclog” certain diseased heart arteries from the inside out. A simple food supplement sold in Japan may have helped reverse a dangerous form of [...]
New breakthrough against radiation: Korean Scientists create revolutionary shield with nanotechnology
Korean Scientists develop new nanotechnology material capable of reducing radiation impacts in space missions, hospitals, and power plants. The search for more efficient protection technologies in extreme environments has just gained an important advance. Korean [...]
Scientists Just Discovered the Hidden Trick That Keeps Your Cells Alive
A strange bead-like motion inside cells may be the secret to keeping their DNA—and health—in balance. Mitochondria are often described as the power plants of the cell because they produce the energy cells need [...]
Scientists Discover Stem Cells That Could Regrow Teeth and Bone
Scientists just uncovered the cellular “blueprint” that could one day let us regrow real teeth. Researchers at Science Tokyo have uncovered two distinct stem cell lineages that play a central role in forming tooth [...]
Scientists Uncover Fatal Weakness in “Zombie Cells” Linked to Cancer
A newly identified weakness in “zombie” cells may open the door to more precise cancer treatments by turning their own survival strategy against them. A new class of drugs takes advantage of a recently [...]
Bowel and Ovarian Cancers Are Dramatically Rising in Young Adults, Scientists Aren’t Sure Why
Cancer incidence is increasing, especially among younger adults, and current risk factors don’t fully account for the trend. Scientists suggest other underlying causes may be contributing. Cancer patterns in England are shifting in a [...]
New Immune Pathway Could Supercharge mRNA Cancer Vaccines
A surprising backup system in the immune response to mRNA vaccines may hold the key to more effective cancer treatments. The arrival of mRNA vaccines against SARS-CoV-2 in 2020 marked a turning point in the COVID-19 pandemic. Today, [...]
Scientists Discover “Molecular Switch” That Fuels Alzheimer’s Brain Inflammation
A newly identified trigger of brain inflammation could offer a fresh target for slowing Alzheimer’s progression. The brain has its own built-in immune system that identifies threats and responds to them. In Alzheimer’s disease, growing evidence [...]
Molecular Manufacturing: The Future of Nanomedicine – New book from NanoappsMedical Inc.
This book explores the revolutionary potential of atomically precise manufacturing technologies to transform global healthcare, as well as practically every other sector across society. This forward-thinking volume examines how envisaged Factory@Home systems might enable the cost-effective [...]
Forgotten Medicinal Plant Shows Promise in Fighting Dangerous Superbugs
A traditional medicinal plant, tormentil, shows promise against antibiotic-resistant bacteria in laboratory tests. Its compounds work by limiting bacterial growth and boosting antibiotic performance. Before the development of modern antibiotics, plant-based remedies were commonly [...]
NanoMedical Brain/Cloud Interface – Explorations and Implications. A new book from Frank Boehm
New book from Frank Boehm, NanoappsMedical Inc Founder: This book explores the future hypothetical possibility that the cerebral cortex of the human brain might be seamlessly, safely, and securely connected with the Cloud via [...]