If you love spicy food, you are not alone. But scientists are taking a closer look at whether eating a lot of chili peppers could affect your cancer risk.
Could your love of spicy food come with hidden risks? A growing body of research suggests that chili peppers, a staple in many cuisines worldwide, may play a complex role in cancers of the digestive system.
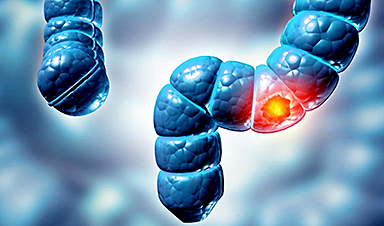
Gastrointestinal cancers, including colorectal, stomach, and esophageal cancers, are among the leading causes of cancer-related illness and death worldwide. Because these diseases are often detected late, researchers are eager to identify lifestyle factors that might help prevent them.
Chili peppers are a major part of diets across the globe. They contain capsaicin, the compound that gives them their heat. Capsaicin has been linked to beneficial effects in lab studies, such as reducing inflammation. At the same time, some research suggests it may also encourage the growth of certain cancer cells, which has made its overall impact unclear.
What the Research Shows
To better understand this, researchers reviewed existing studies on chili pepper consumption and gastrointestinal cancer risk. They analyzed 14 studies involving more than 11,000 people, including over 5,000 cancer cases.
Overall, people who ate the most chili peppers were about 64% more likely to develop gastrointestinal cancers compared to those who ate the least. However, the results were not the same for every type of cancer.
The strongest link was seen with esophageal cancer. People with high chili pepper intake were nearly three times more likely to develop this type of cancer.
In contrast, no statistically significant increase in risk was found for stomach or colorectal cancers, although stomach cancer showed a non-significant trend toward higher risk (about 77% higher in the highest intake group).
The researchers wrote that their findings “suggest that chili pepper is a risk factor for certain GI cancers (e.g., EC).”
Where people live also seemed to make a difference. Higher risks were observed in studies from Asia, Africa, and North America, while studies from Europe and South America actually showed a lower risk. One possible explanation is how much chili pepper people typically consume. In some regions, intake is much higher, which could influence the results.
Regional Differences and Possible Explanations
The team noted that “geographical regions influence the risk of GI cancers,” and said this should be considered when making dietary recommendations.
Scientists also have some ideas about why the esophagus may be more affected. Capsaicin can activate heat and pain receptors, creating the burning sensation associated with spicy foods. Over time, repeated irritation could make the esophagus more vulnerable. Differences in how quickly tissues renew themselves in different parts of the digestive system may also play a role.
Still, the researchers caution that the evidence is not definitive. All of the studies included were observational, meaning they cannot prove that chili peppers directly cause cancer.
More research is needed to understand how much chili pepper is safe and whether moderate consumption carries the same risks as very high intake.
Reference: “Association between chili pepper consumption and risk of gastrointestinal-tract cancers: A meta-analysis” by Changchang Chen, Man Zhang, Xutong Zheng and Hongjuan Lang, 10 October 2022, Frontiers in Nutrition.
DOI: 10.3389/fnut.2022.935865
News – Curated by Amanda Scott, Alias Group Creative
Follow her on Bluesky
UCLA Scientists Uncover a “Hidden Weakness” in Some of the World’s Deadliest Cancers
A new study has uncovered an unexpected vulnerability in some of the deadliest cancers. Researchers at UCLA have identified a previously hidden weakness in some of the most aggressive cancers, pointing to a possible new way [...]
AI-designed universal coronavirus vaccine clears first human trial
Key Takeaways Super-Antigen Technology: Uses AI and machine learning to analyze viral genomes, creating a single vaccine that targets essential features across entire virus families, including coronaviruses and Ebola. Human Trials & Safety: Phase [...]
Researchers Discover a Hidden Vitamin D Problem That Persists Year-Round
A new study suggests that some groups may not experience the expected seasonal boost in vitamin D levels, even during the sunniest months of the year. Many people assume that spending more time outdoors [...]
Researchers Solve the Mystery Behind a Billion-Dollar Dental Implant Disease
Researchers have uncovered why a common and costly dental implant infection often resists antibiotics. Dental implants have helped tens of millions of people regain a full set of stable, functional teeth, something traditional dentures [...]
Nanoparticles inspired by lung fluid improve therapies targeting respiratory system
The CIC biomaGUNE Center for Cooperative Research in Biomaterials has developed pulmonary surfactant nanoparticles (the blend of lipids and proteins that line the alveoli and enables breathing), which are encapsulated [...]
Scientists Finally Uncover How a “Forever Chemical” Causes Birth Defects
PFDA, a PFAS “forever chemical,” can cause craniofacial birth defects by disrupting retinoic acid regulation during fetal development, revealing the first clear molecular mechanism behind the link. Researchers have long linked perfluoroalkyl and polyfluoroalkyl substances (PFAS), [...]
Scientists Have Discovered These Deadly Parasites Are Secretly Swapping DNA
Leishmania parasites appear to evolve through widespread genetic exchange, reshaping assumptions about how they adapt and spread. A parasite long thought to spread mostly by cloning itself may be far more genetically dynamic than [...]
Stanford’s Revolutionary New Microscope Reveals Living Cells in Stunning Detail
Stanford researchers have developed a microscope that can show how nanostructures interact inside living cells at the highest resolution achieved so far. The view into living cells just got better. Stanford researchers have merged [...]
What Bundibugyo Ebola vaccines and treatments are under development
By Mariam Sunny and Jennifer Rigby May 29 (Reuters) – Global health authorities are racing to identify medical options to help contain an Ebola outbreak in eastern Democratic Republic of Congo, linked to the [...]
Why More People in Their 30s Are Suddenly Getting Colon Cancer
A major Swiss study found that colorectal cancer is becoming increasingly common in adults under 50, even as rates decline in older age groups. Researchers in Switzerland have identified a concerning trend: while colorectal [...]
Researchers Compare MS Models to Human Tissue in Search for Better Therapies
Researchers identified key differences between two widely used multiple sclerosis models, showing how each can better study myelin damage, immune responses, and repair. The findings may improve efforts to develop treatments that restore lost [...]
Scientists Discover Genetic “Off Switch” That Supercharges CAR T Cells Against Cancer
A new study reveals a possible way to make CAR T-cell therapy more durable and effective by targeting a single gene-regulating protein. CAR T-cell therapy is widely seen as a breakthrough in personalized cancer [...]
New Vitamin B12-Based Therapy Could Change How Brain Cancer Is Treated
Researchers have identified a vitamin B12–based compound that appears capable of crossing the blood–brain barrier and selectively accumulating in glioblastoma tissue. For decades, one of the biggest problems in brain cancer treatment has had [...]
Simple Fiber Supplement Cuts Knee Arthritis Pain in Just 6 Weeks, Study Finds
A daily inulin supplement may help reduce knee osteoarthritis pain while revealing a possible link between gut health, muscle function, and pain sensitivity. For millions of people living with knee osteoarthritis, managing chronic pain [...]
This Common Vitamin May Help Stop Prediabetes From Turning Into Diabetes
Vitamin D may help prevent type 2 diabetes in people with specific genetic variations, offering a possible path toward personalized diabetes prevention. More than 40% of U.S. adults have prediabetes, a condition in which [...]
Ebola, hantavirus: Is the world prepared for the next pandemic?
Funding cuts to health research and a growing antivaccine movement are making it harder than ever to respond to viruses. The World Health Organization (WHO) has declared that an Ebola outbreak in Uganda and [...]