A key property needed for the effectiveness of CELMoD drugs, a type of protein degrader, has been discovered.
Scripps Research Institute scientists have discovered a crucial feature that is necessary for CELMoDs, a promising new class of cancer drugs, to work effectively.
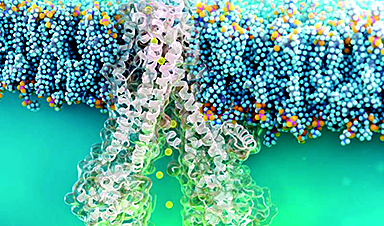
CELMoDs are a new class of cancer drugs that function by binding to cereblon, a regulatory protein, which causes the degradation of proteins that drive cancer. Researchers found that for CELMoDs to work effectively, they must cause a specific shape change in cereblon upon binding. This discovery, recently published in the journal Science, allows for the reliable design of effective CELMoDs.
“There are a lot of research groups that have spent considerable time making drugs that bind very tightly to cereblon, but have then scratched their heads in puzzlement that these drugs fail to work,” says study senior author Gabriel Lander, Ph.D., professor in the Department of Integrative Structural and Computational Biology at Scripps Research.
Cereblon works as part of a major protein-disposal system in cells. This system tags targeted proteins with molecules called ubiquitin, which mark the proteins for destruction by roving protein-breaking complexes known as proteasomes. The ubiquitin-proteasome system is used not only to destroy abnormal or damaged proteins, but also to help regulate the levels of some normal proteins. Cereblon is one of the hundreds of “adaptors” used by the ubiquitin-proteasome system to guide the ubiquitin-tagging process toward specific sets of target proteins.
Scientists now recognize that some cancer drugs, including the best-selling myeloma drug lenalidomide (Revlimid), happen to work by binding to cereblon. They do so in a way that forces the ubiquitin-tagging, and consequent destruction, of key proteins that promote cell division—proteins that couldn’t be targeted easily with traditional drugs. Inspired in part by that recognition, drug companies have begun developing cereblon-binding drugs—CELMoDs, also called protein-degradation drugs—that will work even better against myeloma and other cancers.
One enduring problem for the field has been the fact that some of these drugs bind tightly to cereblon, yet fail to cause sufficient degradation of their protein targets. Understanding why this happens has been difficult. Scientists have wanted to use high-resolution imaging methods to map cereblon’s atomic structure and study its dynamics when bound by CELMoDs. But cereblon is a relatively fragile protein that has been hard to capture with such imaging methods.
In the study, Watson spent more than a year devising a recipe for stabilizing cereblon in association with a ubiquitin-system partner protein, in order to image it with low-temperature electron microscopy (cryo-EM). In this way, he was able ultimately to resolve the cereblon structure at a near-atomic scale. Watson also imaged the cereblon-partner complex with CELMoD compounds and target proteins.
The structural data revealed that CELMoDs must bind to cereblon in a way that changes its shape, or conformation. Cereblon, the researchers determined, has a default “open” conformation, but must be switched to a particular “closed” conformation for the ubiquitin-tagging of target proteins.
The main significance of the finding is that drug companies developing CELMoDs now have a much better idea of what their candidate drugs must do to be effective.
“Companies have been developing cereblon-binding protein-degradation drugs that they can see are better degraders, but they didn’t know this was because the drugs are better at driving this closed conformation,” Watson says. “So now they know, and they can test their drugs for this key property.”
Watson’s breakthrough recipe for stabilizing cereblon in preparation for cryo-EM imaging also is now being adopted widely by researchers in this field.
Lander says his lab hopes now to facilitate the development of protein-degradation drugs that work by binding to other ubiquitin-proteasome adaptor proteins besides cereblon. As he notes, the big attraction of the protein-degradation drug strategy is that it can be used to hit virtually any disease-relevant protein, including the very large class of proteins that can’t be targeted with traditional drugs.
News
New breakthrough against radiation: Korean Scientists create revolutionary shield with nanotechnology
Korean Scientists develop new nanotechnology material capable of reducing radiation impacts in space missions, hospitals, and power plants. The search for more efficient protection technologies in extreme environments has just gained an important advance. Korean [...]
Scientists Just Discovered the Hidden Trick That Keeps Your Cells Alive
A strange bead-like motion inside cells may be the secret to keeping their DNA—and health—in balance. Mitochondria are often described as the power plants of the cell because they produce the energy cells need [...]
Scientists Discover Stem Cells That Could Regrow Teeth and Bone
Scientists just uncovered the cellular “blueprint” that could one day let us regrow real teeth. Researchers at Science Tokyo have uncovered two distinct stem cell lineages that play a central role in forming tooth [...]
Scientists Uncover Fatal Weakness in “Zombie Cells” Linked to Cancer
A newly identified weakness in “zombie” cells may open the door to more precise cancer treatments by turning their own survival strategy against them. A new class of drugs takes advantage of a recently [...]
Bowel and Ovarian Cancers Are Dramatically Rising in Young Adults, Scientists Aren’t Sure Why
Cancer incidence is increasing, especially among younger adults, and current risk factors don’t fully account for the trend. Scientists suggest other underlying causes may be contributing. Cancer patterns in England are shifting in a [...]
New Immune Pathway Could Supercharge mRNA Cancer Vaccines
A surprising backup system in the immune response to mRNA vaccines may hold the key to more effective cancer treatments. The arrival of mRNA vaccines against SARS-CoV-2 in 2020 marked a turning point in the COVID-19 pandemic. Today, [...]
Scientists Discover “Molecular Switch” That Fuels Alzheimer’s Brain Inflammation
A newly identified trigger of brain inflammation could offer a fresh target for slowing Alzheimer’s progression. The brain has its own built-in immune system that identifies threats and responds to them. In Alzheimer’s disease, growing evidence [...]
Molecular Manufacturing: The Future of Nanomedicine – New book from NanoappsMedical Inc.
This book explores the revolutionary potential of atomically precise manufacturing technologies to transform global healthcare, as well as practically every other sector across society. This forward-thinking volume examines how envisaged Factory@Home systems might enable the cost-effective [...]
Forgotten Medicinal Plant Shows Promise in Fighting Dangerous Superbugs
A traditional medicinal plant, tormentil, shows promise against antibiotic-resistant bacteria in laboratory tests. Its compounds work by limiting bacterial growth and boosting antibiotic performance. Before the development of modern antibiotics, plant-based remedies were commonly [...]
NanoMedical Brain/Cloud Interface – Explorations and Implications. A new book from Frank Boehm
New book from Frank Boehm, NanoappsMedical Inc Founder: This book explores the future hypothetical possibility that the cerebral cortex of the human brain might be seamlessly, safely, and securely connected with the Cloud via [...]
New Research Finds Shocking Link Between Chili Peppers and Cancer
If you love spicy food, you are not alone. But scientists are taking a closer look at whether eating a lot of chili peppers could affect your cancer risk. Could your love of spicy [...]
New book from Nanoappsmedical Inc. – Global Health Care Equivalency
A new book by Frank Boehm, NanoappsMedical Inc. Founder. This groundbreaking volume explores the vision of a Global Health Care Equivalency (GHCE) system powered by artificial intelligence and quantum computing technologies, operating on secure [...]
Scientists Create “Neurobots” – Living Machines With Their Own Nervous Systems
Neurobots—xenobots with neurons—show self-organized nervous systems and enhanced behaviors, revealing new insights into how biology builds functional structures. In 2020, researchers at Tufts University developed tiny living structures known as xenobots using frog cells. These microscopic organisms [...]
Our books now available worldwide!
Online Sellers other than Amazon, Routledge, and IOPP Indigo Global Health Care Equivalency in the Age of Nanotechnology, Nanomedicine and Artifcial Intelligence Global Health Care Equivalency In The Age Of Nanotechnology, Nanomedicine And Artificial [...]
Amazonian Chocolate Could Become the Next Superfood, Scientists Say
New research into Amazonian cocoa reveals that its value may extend beyond flavor alone. Chocolate from the Amazon is already known worldwide for its distinctive taste, but new research suggests it may offer even [...]
Nanobody repairs misfolded CFTR inside cells, boosting function in cystic fibrosis
A tiny antibody component could fundamentally transform the treatment of cystic fibrosis: For the first time, researchers have succeeded in developing a so-called nanobody that penetrates directly into human cells and can repair the [...]