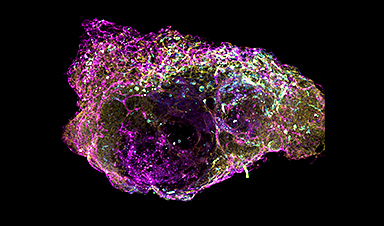
Researchers at Oxford University and the University of Birmingham have made a major breakthrough in cancer treatment by creating the first human bone marrow "organoids" that accurately replicate the key features of human bone marrow. The technology, which is the subject of a patent application filed by the University of Birmingham Enterprise, enables the simultaneous screening of multiple anti-cancer drugs and the testing of personalized treatments for individual cancer patients.
The organoids, which are described in a study recently published in the journal Cancer Discovery, closely mimic the cellular, molecular, and architectural features of myelopoietic (blood cell-producing) bone marrow.
The research also showed that the organoids provide a micro-environment that can accept and support the survival of cells from patients with blood malignancies, including multiple myeloma cells, which are notoriously difficult to maintain outside the human body.
This life-like architecture enabled the team to study how the cells in the bone marrow interact to support normal blood cell production, and how this is disturbed in bone marrow fibrosis (myelofibrosis), where scar tissue builds up in the bone marrow, causing bone marrow failure. Bone marrow fibrosis can develop in patients with certain types of blood cancers and remains incurable.
Senior study author Professor Bethan Psaila, a hematology medical doctor as well as a Research Group Leader at the Radcliffe Department of Medicine, University of Oxford, said "To properly understand how and why blood cancers develop, we need to use experimental systems that closely resemble how real human bone marrow works, which we haven't really had before. It's really exciting to now have this terrific system, as finally, we are able to study cancer directly using cells from our patients, rather than relying on animal models or other simpler systems that do not properly show us how the cancer is developing in the bone marrow in actual patients."
Dr. Khan also added, "This is a huge step forward, enabling insights into the growth patterns of cancer cells and potentially a more personalized approach to treatment. We now have a platform that we can use to test drugs on a 'personalized medicine' basis.
"Having developed and validated the model is the first crucial step, and in our ongoing collaborative work we will be working with others to better understand how the bone marrow works in healthy people, and what goes wrong when they have blood diseases."
Dr. Psaila added, "We hope that this new technique will help accelerate the discovery and testing of new blood cancer treatments, getting improved drugs for our patients to clinical trials faster."
News
Why More People in Their 30s Are Suddenly Getting Colon Cancer
A major Swiss study found that colorectal cancer is becoming increasingly common in adults under 50, even as rates decline in older age groups. Researchers in Switzerland have identified a concerning trend: while colorectal [...]
Researchers Compare MS Models to Human Tissue in Search for Better Therapies
Researchers identified key differences between two widely used multiple sclerosis models, showing how each can better study myelin damage, immune responses, and repair. The findings may improve efforts to develop treatments that restore lost [...]
Scientists Discover Genetic “Off Switch” That Supercharges CAR T Cells Against Cancer
A new study reveals a possible way to make CAR T-cell therapy more durable and effective by targeting a single gene-regulating protein. CAR T-cell therapy is widely seen as a breakthrough in personalized cancer [...]
New Vitamin B12-Based Therapy Could Change How Brain Cancer Is Treated
Researchers have identified a vitamin B12–based compound that appears capable of crossing the blood–brain barrier and selectively accumulating in glioblastoma tissue. For decades, one of the biggest problems in brain cancer treatment has had [...]
Simple Fiber Supplement Cuts Knee Arthritis Pain in Just 6 Weeks, Study Finds
A daily inulin supplement may help reduce knee osteoarthritis pain while revealing a possible link between gut health, muscle function, and pain sensitivity. For millions of people living with knee osteoarthritis, managing chronic pain [...]
This Common Vitamin May Help Stop Prediabetes From Turning Into Diabetes
Vitamin D may help prevent type 2 diabetes in people with specific genetic variations, offering a possible path toward personalized diabetes prevention. More than 40% of U.S. adults have prediabetes, a condition in which [...]
Ebola, hantavirus: Is the world prepared for the next pandemic?
Funding cuts to health research and a growing antivaccine movement are making it harder than ever to respond to viruses. The World Health Organization (WHO) has declared that an Ebola outbreak in Uganda and [...]
May 2026 Healthcare News and Trends: Market Signals That Matter
Artificial intelligence is dominating headlines, telehealth has settled into a new normal, and digital health continues to promise transformation. However, much of what is being discussed in healthcare today reflects potential rather than reality. [...]
Scientists Rewire Donor Stem Cells To Outsmart Aggressive Blood Cancers
Researchers have tested a gene-edited stem cell transplant designed to shield healthy blood-forming cells from powerful cancer-targeting immunotherapies. For patients with highly aggressive blood cancers, stem cell transplantation can offer a rare chance at [...]
Recent Digital Health Trends, Insights and News – May 2026
Last month marked continued progress as digital health moves into its next phase — from AI expanding into drug discovery and core infrastructure to new federal pathways accelerating device access and home-based care. Together, [...]
Cancer Mystery Solved: Scientists Discover How Melanoma Becomes “Immortal”
Scientists have uncovered a previously overlooked mechanism that may help melanoma cells become effectively “immortal.” Cancer cells face a major problem before they can become deadly: They have to figure out how to stop [...]
How Visual Neurons Organize Thousands of Synaptic Inputs
Summary: A new study uncovered the organizational rules that determine how neurons in the primary visual cortex process information. By imaging both the cell bodies (soma) and the individual synapses (on dendritic spines) of [...]
Scientists Just Found a Surprising Way To Destroy “Forever Chemicals”
Scientists have uncovered a new mechanism that may help break down highly persistent PFAS pollutants. PFAS have earned the nickname “forever chemicals” for a reason. These industrial compounds are so chemically durable that they [...]
Scientists Discover Cheap Material That Kills Deadly Superbugs
A new sulfur-rich antimicrobial polymer shows strong effectiveness against fungal and bacterial pathogens and may offer an affordable solution to antimicrobial resistance. Antimicrobial resistance is creating growing challenges for both healthcare and food production, [...]
What to Know About Cicada, or BA.3.2, the Latest SARS-CoV-2 Variant Under Monitoring
Like periodical cicadas, the insects for which it is nicknamed, SARS-CoV-2 Omicron subvariant BA.3.2 is only just beginning to emerge after lying low for an extended period since it first appeared. Although it was [...]
Scientists Say This Simple Supplement May Actually Reverse Heart Disease
Scientists in Japan say a common supplement may actually help “unclog” certain diseased heart arteries from the inside out. A simple food supplement sold in Japan may have helped reverse a dangerous form of [...]