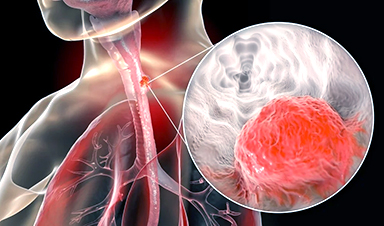
Among the total number of deaths caused by different types of cancer, esophageal cancer is the sixth most significant. Several conventional treatments, such as radiotherapy, chemotherapy, and surgery have multiple side effects, including off-target toxicity and multidrug resistance (MDR).
Another strategy for esophageal cancer treatment is chemo-photodynamic therapy, the efficacy of which is limited by its inability to target tumors, lack of suitable microenvironment for photodynamic therapy (PDT), and tendency to cause adverse side effects.
Scientists sought to address these limitations of the existing therapies and developed a novel theranostic nanoplatform, namely, GCDs-Ce6/Pt-EGF, which has been found to be effective against esophageal cancer. This study has been recently published in Biomedicine & Pharmacotherapy.
Conventional Treatments of Esophageal Cancer
The majority of the available treatments for esophageal cancers come with some limitations. For instance, as this type of cancer is prone to metastasis, surgery cannot completely remove the tumor. In the case of radiotherapy, the narrow dose window limits its purpose. Low-dose radionuclides have limited tumor cell killing ability, while high dosage can affect healthy cells as well.
Although chemotherapy, using Cisplatin or Doxorubicin, can effectively eliminate tumor cells with metastasis and has a superior anti-tumor effect, it often severely damages the kidney and liver of the patient. Combinational therapy, such as chemoradiation with surgery, was effective against esophageal cancer, but this therapy showed high in-hospital mortality.
Two of the limitations associated with photothermal therapy and oxidative therapy are the recurrence of tumor cells and damage caused to off-target non-cancerous cells as well. PDT is effective against different types of cancers, such as breast, prostate, liver, and esophagus, with a better biosafety effect. However, its effectiveness is compromised by abundant glutathione (GSH) in the tumor microenvironment and hypoxia.
Nanotechnology-based Cancer Treatments
Nanoparticles are widely used in biomedical research, owing to their nanoscale dimension (1–100 nm) and multiple unique properties. Carbon nanodots are a type of carbon nanoparticle that is applied for fluorescence sensing, bioimaging, and drug delivery. The development of tumor-targeted drug delivery systems is essential to facilitate tumor-specific treatment without adversely affecting the normal cells.
Drugs are often modified to identify tumor cells by recognizing specific receptors expressed in them. In many types of cancers, including esophageal cancer, the epidermal growth factor receptor (EGFR) is found to be overexpressed. Compared to healthy individuals, esophageal cancer patients exhibit a significantly higher expression of EGFR protein in the mucosa. Hence, this receptor has been utilized as a key target for anti-tumor drug delivery.
A Novel Theranostic Nanoplatform for Esophageal Cancer Treatment
Recently, scientists have developed an all-in-one theranostic nanoplatform, known as GCDs-Ce6/Pt-EGF for esophageal cancer treatment. This nanoplatform utilized green fluorescence carbon dots (GCDs), which were synthesized using p-aminosalicylic acid and p-aminobenzamide with a molar ratio of 1:1 at 200℃ for 6 hours, via the hydrothermal method.
GCDs were characterized using atomic force microscopy (AFM) and transmission electron microscopy (TEM), which revealed a uniform dispersion of quasi-sphere GCD nanomaterials of 4.72 nm size. The fluorescence quantum yield of GCDs was estimated to be 10.62%. Most importantly, this nanoparticle exhibited excellent optical stability.
To construct the GCDs-Ce6/Pt-EGF nanoplatform, researchers grafted chlorin e6 (Ce6), which is a photosensitizer, chemotherapy agent Pt (IV), and the targeting unit epidermal growth factor (EGF) on GCDs. Here, the drug loading rates of Ce6 and Pt (IV) were estimated to be 8.53% and 19.36%, respectively. The drug loading capacity of GCDs-Ce6/Pt-EGF nanoplatform was observed to be significantly more than other nanoplatforms.
Post irradiation at 660 nm wavelength, photosensitizer Ce6 induced cell death by generating reactive oxygen species (ROS). This phenomenon induced tumor cell apoptosis. Both in vitro and in vivo studies strongly indicated that the GCDs-Ce6/Pt-EGF exhibited superior photodynamic properties and could be effectively applied for esophageal tumor imaging as well as the elimination of esophageal cancer cells (therapeutic effect).
The mechanism driving the GCDs-Ce6/Pt-EGF nanoplatform is the targeting of esophageal cancer cells, bearing EGFR, and penetration of the tumor cells. After internalization within the tumor cells, Pt(IV) gets converted to Pt(II) by intracellular GSH, which ultimately kills tumor cells.
Interestingly, this study revealed that GCDs-Ce6/Pt-EGF displayed better anti-tumor effects compared to Cisplatin. Researchers stated that this nanomedicine could not only restrict tumor cell migration but also target tumor cells by recognizing EGF receptors. Other important aspects of this theranostic nanoplatform are direct cell killing capacity by Pt(II) and laser irradiation.
The GCDs-Ce6/Pt-EGF nanoplatform displayed excellent biosafety, as it rendered negligible cytotoxicity to normal esophageal cells. This could be due to three reasons, i.e., superior tumor targeting capability that reduces off-target toxicity, the release of toxic platinum only in GSH-rich tumor microenvironment, and Ce6 induced PDT effect with laser irradiation. Scientists are optimistic that utilizing all-in-one GCDs-Ce6/Pt-EGF theranostic nanoplatform could be beneficial for treating esophageal cancer patients.
News
This Common Vitamin May Help Stop Prediabetes From Turning Into Diabetes
Vitamin D may help prevent type 2 diabetes in people with specific genetic variations, offering a possible path toward personalized diabetes prevention. More than 40% of U.S. adults have prediabetes, a condition in which [...]
Ebola, hantavirus: Is the world prepared for the next pandemic?
Funding cuts to health research and a growing antivaccine movement are making it harder than ever to respond to viruses. The World Health Organization (WHO) has declared that an Ebola outbreak in Uganda and [...]
May 2026 Healthcare News and Trends: Market Signals That Matter
Artificial intelligence is dominating headlines, telehealth has settled into a new normal, and digital health continues to promise transformation. However, much of what is being discussed in healthcare today reflects potential rather than reality. [...]
Scientists Rewire Donor Stem Cells To Outsmart Aggressive Blood Cancers
Researchers have tested a gene-edited stem cell transplant designed to shield healthy blood-forming cells from powerful cancer-targeting immunotherapies. For patients with highly aggressive blood cancers, stem cell transplantation can offer a rare chance at [...]
Recent Digital Health Trends, Insights and News – May 2026
Last month marked continued progress as digital health moves into its next phase — from AI expanding into drug discovery and core infrastructure to new federal pathways accelerating device access and home-based care. Together, [...]
Cancer Mystery Solved: Scientists Discover How Melanoma Becomes “Immortal”
Scientists have uncovered a previously overlooked mechanism that may help melanoma cells become effectively “immortal.” Cancer cells face a major problem before they can become deadly: They have to figure out how to stop [...]
How Visual Neurons Organize Thousands of Synaptic Inputs
Summary: A new study uncovered the organizational rules that determine how neurons in the primary visual cortex process information. By imaging both the cell bodies (soma) and the individual synapses (on dendritic spines) of [...]
Scientists Just Found a Surprising Way To Destroy “Forever Chemicals”
Scientists have uncovered a new mechanism that may help break down highly persistent PFAS pollutants. PFAS have earned the nickname “forever chemicals” for a reason. These industrial compounds are so chemically durable that they [...]
Scientists Discover Cheap Material That Kills Deadly Superbugs
A new sulfur-rich antimicrobial polymer shows strong effectiveness against fungal and bacterial pathogens and may offer an affordable solution to antimicrobial resistance. Antimicrobial resistance is creating growing challenges for both healthcare and food production, [...]
What to Know About Cicada, or BA.3.2, the Latest SARS-CoV-2 Variant Under Monitoring
Like periodical cicadas, the insects for which it is nicknamed, SARS-CoV-2 Omicron subvariant BA.3.2 is only just beginning to emerge after lying low for an extended period since it first appeared. Although it was [...]
Scientists Say This Simple Supplement May Actually Reverse Heart Disease
Scientists in Japan say a common supplement may actually help “unclog” certain diseased heart arteries from the inside out. A simple food supplement sold in Japan may have helped reverse a dangerous form of [...]
New breakthrough against radiation: Korean Scientists create revolutionary shield with nanotechnology
Korean Scientists develop new nanotechnology material capable of reducing radiation impacts in space missions, hospitals, and power plants. The search for more efficient protection technologies in extreme environments has just gained an important advance. Korean [...]
Scientists Just Discovered the Hidden Trick That Keeps Your Cells Alive
A strange bead-like motion inside cells may be the secret to keeping their DNA—and health—in balance. Mitochondria are often described as the power plants of the cell because they produce the energy cells need [...]
Scientists Discover Stem Cells That Could Regrow Teeth and Bone
Scientists just uncovered the cellular “blueprint” that could one day let us regrow real teeth. Researchers at Science Tokyo have uncovered two distinct stem cell lineages that play a central role in forming tooth [...]
Scientists Uncover Fatal Weakness in “Zombie Cells” Linked to Cancer
A newly identified weakness in “zombie” cells may open the door to more precise cancer treatments by turning their own survival strategy against them. A new class of drugs takes advantage of a recently [...]
Bowel and Ovarian Cancers Are Dramatically Rising in Young Adults, Scientists Aren’t Sure Why
Cancer incidence is increasing, especially among younger adults, and current risk factors don’t fully account for the trend. Scientists suggest other underlying causes may be contributing. Cancer patterns in England are shifting in a [...]