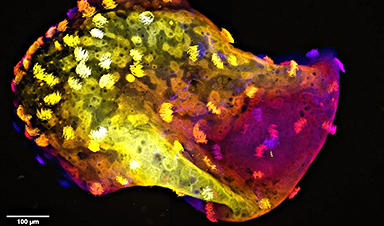
Just what is COVID capable of doing to the human brain?
What they saw explained a lot: An “excessive number” of synapses, or connections between brain cells that allow them to communicate, were eliminated during the course of the disease—“more than you would expect to see in a normal brain,” the authors wrote in an Oct. 27 article on academic news site The Conversation.
In a process known as “pruning,” normal brains get rid of a certain amount of inactive synapses when they’re no longer needed, to make way for new ones. But the infected mini brains showed unnecessary and inordinate levels of the clean-up process, similar to the level seen in neurological disorders like schizophrenia, Alzheimer’s, and Parkinson’s disease, according to the authors.
What researchers witnessed may explain why many Long COVID sufferers report neurological symptoms, and why COVID seems to increase the risk of developing some neurological disorders.
It’s well established that those who’ve had COVID are at an increased risk for complications like stroke, memory problems, depression, anxiety, and migraines. More than a third of those who’ve had COVID report neurologic symptoms, according to a February article in Therapeutic Advances in Chronic Disease.
And it’s well known that some Long COVID sufferers experience neurologic symptoms like tremors, issues with movement, involuntary muscle contractions, seizures, hearing and vision issues, balance and coordination problems, and other Parkinson’s disease-like symptoms. The most frequent neurological symptoms of Long COVID include “brain fog,” headache, confusion, sleep disorders, mood disorders, issues with smell or taste, and dysautonomia, a disorder of the autonomic nervous system that can involve fainting, drops in blood pressure when standing, rapid heart rate, and other issues with involuntary bodily functions.
Nearly 20% of American adults who’ve had COVID—an estimated 50 million—report having Long COVID symptoms after their infection resolves, according to data collected by the U.S. Census Bureau this summer.
Long COVID is roughly defined as symptoms that persist or appear long after the initial COVID infection is gone, but a consensus definition has not yet been broadly accepted.
Many experts contend that long COVID is best defined as a chronic-fatigue-syndrome-like condition that develops after COVID illness, similar to other post-viral syndromes like those that can occur after infection with herpes, Lyme disease, and even Ebola. Other post-COVID complications like post-intensive-care syndrome should not be defined as long COVID, they say.
News
Scientists Uncover Fatal Weakness in “Zombie Cells” Linked to Cancer
A newly identified weakness in “zombie” cells may open the door to more precise cancer treatments by turning their own survival strategy against them. A new class of drugs takes advantage of a recently [...]
Bowel and Ovarian Cancers Are Dramatically Rising in Young Adults, Scientists Aren’t Sure Why
Cancer incidence is increasing, especially among younger adults, and current risk factors don’t fully account for the trend. Scientists suggest other underlying causes may be contributing. Cancer patterns in England are shifting in a [...]
New Immune Pathway Could Supercharge mRNA Cancer Vaccines
A surprising backup system in the immune response to mRNA vaccines may hold the key to more effective cancer treatments. The arrival of mRNA vaccines against SARS-CoV-2 in 2020 marked a turning point in the COVID-19 pandemic. Today, [...]
Scientists Discover “Molecular Switch” That Fuels Alzheimer’s Brain Inflammation
A newly identified trigger of brain inflammation could offer a fresh target for slowing Alzheimer’s progression. The brain has its own built-in immune system that identifies threats and responds to them. In Alzheimer’s disease, growing evidence [...]
Molecular Manufacturing: The Future of Nanomedicine – New book from NanoappsMedical Inc.
This book explores the revolutionary potential of atomically precise manufacturing technologies to transform global healthcare, as well as practically every other sector across society. This forward-thinking volume examines how envisaged Factory@Home systems might enable the cost-effective [...]
Forgotten Medicinal Plant Shows Promise in Fighting Dangerous Superbugs
A traditional medicinal plant, tormentil, shows promise against antibiotic-resistant bacteria in laboratory tests. Its compounds work by limiting bacterial growth and boosting antibiotic performance. Before the development of modern antibiotics, plant-based remedies were commonly [...]
NanoMedical Brain/Cloud Interface – Explorations and Implications. A new book from Frank Boehm
New book from Frank Boehm, NanoappsMedical Inc Founder: This book explores the future hypothetical possibility that the cerebral cortex of the human brain might be seamlessly, safely, and securely connected with the Cloud via [...]
New Research Finds Shocking Link Between Chili Peppers and Cancer
If you love spicy food, you are not alone. But scientists are taking a closer look at whether eating a lot of chili peppers could affect your cancer risk. Could your love of spicy [...]
New book from Nanoappsmedical Inc. – Global Health Care Equivalency
A new book by Frank Boehm, NanoappsMedical Inc. Founder. This groundbreaking volume explores the vision of a Global Health Care Equivalency (GHCE) system powered by artificial intelligence and quantum computing technologies, operating on secure [...]
Scientists Create “Neurobots” – Living Machines With Their Own Nervous Systems
Neurobots—xenobots with neurons—show self-organized nervous systems and enhanced behaviors, revealing new insights into how biology builds functional structures. In 2020, researchers at Tufts University developed tiny living structures known as xenobots using frog cells. These microscopic organisms [...]
Our books now available worldwide!
Online Sellers other than Amazon, Routledge, and IOPP Indigo Global Health Care Equivalency in the Age of Nanotechnology, Nanomedicine and Artifcial Intelligence Global Health Care Equivalency In The Age Of Nanotechnology, Nanomedicine And Artificial [...]
Amazonian Chocolate Could Become the Next Superfood, Scientists Say
New research into Amazonian cocoa reveals that its value may extend beyond flavor alone. Chocolate from the Amazon is already known worldwide for its distinctive taste, but new research suggests it may offer even [...]
Nanobody repairs misfolded CFTR inside cells, boosting function in cystic fibrosis
A tiny antibody component could fundamentally transform the treatment of cystic fibrosis: For the first time, researchers have succeeded in developing a so-called nanobody that penetrates directly into human cells and can repair the [...]
20-Year Study Finds Daily Multivitamins Don’t Extend Lifespan
A large, decades-long study of over 390,000 U.S. adults challenges a widespread assumption about daily multivitamins. Multivitamins are a daily habit for millions of Americans, often taken with the expectation that they will extend [...]
Novel Investment Paradigms for Regenerative Healthcare Ecosystems
Introduction The transition toward regenerative healthcare ecosystems—anchored in wellness optimization, disease prevention, eradication strategies, and healthy longevity—necessitates a structural reconfiguration of capital architectures, governance models, and incentive design. Regenerative healthcare, by definition, transcends episodic [...]
What If Consciousness Exists Beyond Your Brain
Scientists still don’t know how consciousness emerges from the brain. New ideas suggest it may not emerge at all, but instead be a basic feature of reality. Is consciousness produced by the brain, or [...]