| Using nanotechnology that enabled mRNA-based COVID-19 vaccines, a new approach to gene therapy may improve how physicians treat inherited forms of blindness. | |
| A collaborative team of researchers with Oregon Health & Science University and Oregon State University have developed an approach that uses lipid nanoparticles — tiny, lab-made balls of fat — to deliver strands of messenger ribonucleic acid, or mRNA, inside the eye. To treat blindness, the mRNA will be designed to create proteins that edit vision-harming gene mutations. | |
| In a study published in Science Advances (“Peptide-guided lipid nanoparticles deliver mRNA to the neural retina of rodents and nonhuman primates”), the team demonstrates how its lipid nanoparticle delivery system targets light-sensitive cells in the eye, called photoreceptors, in both mice and nonhuman primates. The system’s nanoparticles are coated with a peptide that the researchers identified as being attracted to photoreceptors. | |
| “Our peptide is like a zip code, and the lipid nanoparticles are similar to an envelope that sends gene therapy in the mail,” explained the study’s corresponding author, Gaurav Sahay, Ph.D., an associate professor in the OSU College of Pharmacy who also has a joint research appointment at the OHSU Casey Eye Institute. “The peptide ensures mRNA is precisely delivered to photoreceptors — cells that we haven’t been able to target with lipid nanoparticles until now.” | |
| “More than 250 genetic mutations have been linked to inherited retinal diseases, but only one has an approved gene therapy,” added study co-author Renee Ryals, Ph.D., an assistant professor of ophthalmology in the OHSU School of Medicine and a scientist at the OHSU Casey Eye Institute. “Improving the technologies used for gene therapy can provide more treatment options to prevent blindness. Our study’s findings show that lipid nanoparticles could help us do just that.” |
| In 2017, the Food and Drug Administration approved the first gene therapy to treat an inherited form of blindness. Many patients have experienced improved vision and have been spared blindness after receiving the therapy, which is sold under the brand name Luxturna. It uses a modified version of the adeno-associated virus, or AAV, to deliver gene-revising molecules. | |
| Today’s gene therapies largely rely on AAV, but it has some limitations. The virus is relatively small and can’t physically contain gene-editing machinery for some complex mutations. And AAV-based gene therapy can only deliver DNA, which results in the continual creation of gene-editing molecules that may lead to unintended genetic edits. | |
| Lipid nanoparticles are a promising alternative because they don’t have size constraints like AAV. Additionally, lipid nanoparticles can deliver mRNA, which only keeps gene-editing machinery active for a short period of time, so could prevent off-target edits. The potential of lipid nanoparticles was further proved by the success of mRNA-based COVID-19 vaccines, which also use lipid nanoparticles to deliver mRNA. They also were the first vaccines to be authorized for COVID-19 in the United States, thanks to the speed and volume at which they can be manufactured. | |
| In this study, Sahay, Ryals and colleagues demonstrated that a peptide-covered lipid nanoparticle shell can be directed toward photoreceptor cells in the retina, tissue in the back of the eye that enables sight. As a first proof of concept, mRNA with instructions to make green fluorescent protein was placed inside nanoparticles. | |
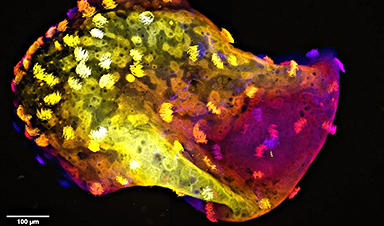
| After injecting this nanoparticle-based gene therapy model into the eyes of mice and nonhuman primates, the research team used a variety of imaging techniques to examine the treated eyes. The animals’ retinal tissue glowed green, illustrating that the lipid nanoparticle shell reached photoreceptors and that the mRNA it delivered successfully entered the retina and created green fluorescent protein. This research marks the first time that lipid nanoparticles are known to have targeted photoreceptors in a nonhuman primate. | |
| The scientists are currently working on follow-up research to quantify how much of the green fluorescent protein is expressed in animal retinal models. They’re also working to develop a therapy with mRNA that carries the code for gene-editing molecules. |
News
New breakthrough against radiation: Korean Scientists create revolutionary shield with nanotechnology
Korean Scientists develop new nanotechnology material capable of reducing radiation impacts in space missions, hospitals, and power plants. The search for more efficient protection technologies in extreme environments has just gained an important advance. Korean [...]
Scientists Just Discovered the Hidden Trick That Keeps Your Cells Alive
A strange bead-like motion inside cells may be the secret to keeping their DNA—and health—in balance. Mitochondria are often described as the power plants of the cell because they produce the energy cells need [...]
Scientists Discover Stem Cells That Could Regrow Teeth and Bone
Scientists just uncovered the cellular “blueprint” that could one day let us regrow real teeth. Researchers at Science Tokyo have uncovered two distinct stem cell lineages that play a central role in forming tooth [...]
Scientists Uncover Fatal Weakness in “Zombie Cells” Linked to Cancer
A newly identified weakness in “zombie” cells may open the door to more precise cancer treatments by turning their own survival strategy against them. A new class of drugs takes advantage of a recently [...]
Bowel and Ovarian Cancers Are Dramatically Rising in Young Adults, Scientists Aren’t Sure Why
Cancer incidence is increasing, especially among younger adults, and current risk factors don’t fully account for the trend. Scientists suggest other underlying causes may be contributing. Cancer patterns in England are shifting in a [...]
New Immune Pathway Could Supercharge mRNA Cancer Vaccines
A surprising backup system in the immune response to mRNA vaccines may hold the key to more effective cancer treatments. The arrival of mRNA vaccines against SARS-CoV-2 in 2020 marked a turning point in the COVID-19 pandemic. Today, [...]
Scientists Discover “Molecular Switch” That Fuels Alzheimer’s Brain Inflammation
A newly identified trigger of brain inflammation could offer a fresh target for slowing Alzheimer’s progression. The brain has its own built-in immune system that identifies threats and responds to them. In Alzheimer’s disease, growing evidence [...]
Molecular Manufacturing: The Future of Nanomedicine – New book from NanoappsMedical Inc.
This book explores the revolutionary potential of atomically precise manufacturing technologies to transform global healthcare, as well as practically every other sector across society. This forward-thinking volume examines how envisaged Factory@Home systems might enable the cost-effective [...]
Forgotten Medicinal Plant Shows Promise in Fighting Dangerous Superbugs
A traditional medicinal plant, tormentil, shows promise against antibiotic-resistant bacteria in laboratory tests. Its compounds work by limiting bacterial growth and boosting antibiotic performance. Before the development of modern antibiotics, plant-based remedies were commonly [...]
NanoMedical Brain/Cloud Interface – Explorations and Implications. A new book from Frank Boehm
New book from Frank Boehm, NanoappsMedical Inc Founder: This book explores the future hypothetical possibility that the cerebral cortex of the human brain might be seamlessly, safely, and securely connected with the Cloud via [...]
New Research Finds Shocking Link Between Chili Peppers and Cancer
If you love spicy food, you are not alone. But scientists are taking a closer look at whether eating a lot of chili peppers could affect your cancer risk. Could your love of spicy [...]
New book from Nanoappsmedical Inc. – Global Health Care Equivalency
A new book by Frank Boehm, NanoappsMedical Inc. Founder. This groundbreaking volume explores the vision of a Global Health Care Equivalency (GHCE) system powered by artificial intelligence and quantum computing technologies, operating on secure [...]
Scientists Create “Neurobots” – Living Machines With Their Own Nervous Systems
Neurobots—xenobots with neurons—show self-organized nervous systems and enhanced behaviors, revealing new insights into how biology builds functional structures. In 2020, researchers at Tufts University developed tiny living structures known as xenobots using frog cells. These microscopic organisms [...]
Our books now available worldwide!
Online Sellers other than Amazon, Routledge, and IOPP Indigo Global Health Care Equivalency in the Age of Nanotechnology, Nanomedicine and Artifcial Intelligence Global Health Care Equivalency In The Age Of Nanotechnology, Nanomedicine And Artificial [...]
Amazonian Chocolate Could Become the Next Superfood, Scientists Say
New research into Amazonian cocoa reveals that its value may extend beyond flavor alone. Chocolate from the Amazon is already known worldwide for its distinctive taste, but new research suggests it may offer even [...]
Nanobody repairs misfolded CFTR inside cells, boosting function in cystic fibrosis
A tiny antibody component could fundamentally transform the treatment of cystic fibrosis: For the first time, researchers have succeeded in developing a so-called nanobody that penetrates directly into human cells and can repair the [...]