Marla Kott was diagnosed with Stage 4 lung cancer on Nov. 21, 2014. It was her 60th birthday.
"It was not a great day," said Kott, who was was one of thousands of people in Canada diagnosed with lung cancer that year.
The disease accounts for a quarter of cancer deaths, according to the Canadian Cancer Society. The society says the five-year survival rate is 62 per cent for those diagnosed with Stage 1 lung cancer, and drops to three per cent for Stage 4.
It took about a year for Kott to be diagnosed, after undergoing numerous tests to determine what was wrong.
Against the odds, Kott is still going strong nine years later — but the Vancouver resident wishes there had been a way to detect her cancer sooner.
"I might have been able to have surgery and be done with it," she said, imagining scenarios in which the disease was discovered early and fully treated.
Researchers with B.C. Cancer in Vancouver are now working to develop a breath test that could help show signs of cancer earlier, and screen more people, more easily.
"When we exhale, we exhale over 1,000 volatile organic compounds," said team co-lead Dr. Renelle Myers, adding that some of these compounds have the potential to indicate cancer development.
Myers first began studying breath samples in 2020, when she opened what she says is the first clinical breath lab in Canada. When the pandemic hit, her team pivoted from cancer research to looking at the detection of COVID through breath.
"If we can find that fingerprint of an early lung cancer, that will help us screen, much more easily, many, many people around the province and around the world."
Additionally, researchers hope the test will help them understand how changes in the lungs might indicate cancer development in people who have never smoked.
"We are seeing an alarming increase of lung cancer in never-smokers," Myers said.
A study published by B.C. Cancer in June 2023 found that 33 per cent of lung cancer patients in Vancouver had never used tobacco products, and suggested air pollution might be the cause — in particular, a particle called PM2.5, levels of which are higher in B.C. during wildfire season.
AI organizing data
The test researchers are working on uses artificial intelligence to sift through data.
"There's thousands of compounds in a single breath," Myers said, adding that AI helps organize people by age, risk factors and other indicators of cancer.
"Even if our team works 24/7, we couldn't process all the samples required for these large, multi-centre studies with only the system we have now," research team co-lead Dr. Stephen Lam said. "Especially since samples can't be stored for very long once collected."
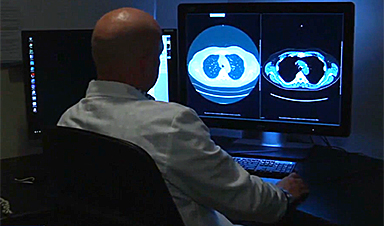
Currently, the best way to diagnose lung cancer is through a CT (computed tomography) scan, Myers said. But other tests, including blood tests, X-rays, MRIs, ultrasounds and biopsies, to name a few, can be part of the determination.
"The majority of patients who are diagnosed with lung cancer are diagnosed at a late stage when they become symptomatic," Myers said.
The team is in the early stages of nationwide clinical study, having collected nearly 300 samples from individuals in Ontario, B.C. and Quebec. The goal is to look at samples from 4,000 people.
They're looking at pulmonary nodules — small clumps of cells in the lungs — that are often benign but can develop into cancer.
Researchers will follow patients over five years to see how those nodules develop and how breath signatures change in turn.
By being able to identify if a nodule is not cancerous, Myers said patients could be given the all clear, and not have to follow up for several months.
"It's powerful in that it could potentially really reduce downstream resource utilization in our health-care system," she said.
News
Why More People in Their 30s Are Suddenly Getting Colon Cancer
A major Swiss study found that colorectal cancer is becoming increasingly common in adults under 50, even as rates decline in older age groups. Researchers in Switzerland have identified a concerning trend: while colorectal [...]
Researchers Compare MS Models to Human Tissue in Search for Better Therapies
Researchers identified key differences between two widely used multiple sclerosis models, showing how each can better study myelin damage, immune responses, and repair. The findings may improve efforts to develop treatments that restore lost [...]
Scientists Discover Genetic “Off Switch” That Supercharges CAR T Cells Against Cancer
A new study reveals a possible way to make CAR T-cell therapy more durable and effective by targeting a single gene-regulating protein. CAR T-cell therapy is widely seen as a breakthrough in personalized cancer [...]
New Vitamin B12-Based Therapy Could Change How Brain Cancer Is Treated
Researchers have identified a vitamin B12–based compound that appears capable of crossing the blood–brain barrier and selectively accumulating in glioblastoma tissue. For decades, one of the biggest problems in brain cancer treatment has had [...]
Simple Fiber Supplement Cuts Knee Arthritis Pain in Just 6 Weeks, Study Finds
A daily inulin supplement may help reduce knee osteoarthritis pain while revealing a possible link between gut health, muscle function, and pain sensitivity. For millions of people living with knee osteoarthritis, managing chronic pain [...]
This Common Vitamin May Help Stop Prediabetes From Turning Into Diabetes
Vitamin D may help prevent type 2 diabetes in people with specific genetic variations, offering a possible path toward personalized diabetes prevention. More than 40% of U.S. adults have prediabetes, a condition in which [...]
Ebola, hantavirus: Is the world prepared for the next pandemic?
Funding cuts to health research and a growing antivaccine movement are making it harder than ever to respond to viruses. The World Health Organization (WHO) has declared that an Ebola outbreak in Uganda and [...]
May 2026 Healthcare News and Trends: Market Signals That Matter
Artificial intelligence is dominating headlines, telehealth has settled into a new normal, and digital health continues to promise transformation. However, much of what is being discussed in healthcare today reflects potential rather than reality. [...]
Scientists Rewire Donor Stem Cells To Outsmart Aggressive Blood Cancers
Researchers have tested a gene-edited stem cell transplant designed to shield healthy blood-forming cells from powerful cancer-targeting immunotherapies. For patients with highly aggressive blood cancers, stem cell transplantation can offer a rare chance at [...]
Recent Digital Health Trends, Insights and News – May 2026
Last month marked continued progress as digital health moves into its next phase — from AI expanding into drug discovery and core infrastructure to new federal pathways accelerating device access and home-based care. Together, [...]
Cancer Mystery Solved: Scientists Discover How Melanoma Becomes “Immortal”
Scientists have uncovered a previously overlooked mechanism that may help melanoma cells become effectively “immortal.” Cancer cells face a major problem before they can become deadly: They have to figure out how to stop [...]
How Visual Neurons Organize Thousands of Synaptic Inputs
Summary: A new study uncovered the organizational rules that determine how neurons in the primary visual cortex process information. By imaging both the cell bodies (soma) and the individual synapses (on dendritic spines) of [...]
Scientists Just Found a Surprising Way To Destroy “Forever Chemicals”
Scientists have uncovered a new mechanism that may help break down highly persistent PFAS pollutants. PFAS have earned the nickname “forever chemicals” for a reason. These industrial compounds are so chemically durable that they [...]
Scientists Discover Cheap Material That Kills Deadly Superbugs
A new sulfur-rich antimicrobial polymer shows strong effectiveness against fungal and bacterial pathogens and may offer an affordable solution to antimicrobial resistance. Antimicrobial resistance is creating growing challenges for both healthcare and food production, [...]
What to Know About Cicada, or BA.3.2, the Latest SARS-CoV-2 Variant Under Monitoring
Like periodical cicadas, the insects for which it is nicknamed, SARS-CoV-2 Omicron subvariant BA.3.2 is only just beginning to emerge after lying low for an extended period since it first appeared. Although it was [...]
Scientists Say This Simple Supplement May Actually Reverse Heart Disease
Scientists in Japan say a common supplement may actually help “unclog” certain diseased heart arteries from the inside out. A simple food supplement sold in Japan may have helped reverse a dangerous form of [...]