In 1988, Richard Lenski, a thirty-one-year-old biologist at UC Irvine, started an experiment. He divided a population of a common bacterium, E. coli, into twelve flasks. Each flask was kept at thirty-seven degrees Celsius, and contained an identical cocktail of water, glucose, and other nutrients. Each day, as the bacteria replicated, Lenski transferred several drops of each cocktail to a new flask, and every so often he stored samples away in a freezer. His goal was to understand the mechanics of evolution. How quickly, effectively, creatively, and consistently do microorganisms improve their reproductive fitness?
Lenski’s flasks produced about six new generations of E. coli a day; the bacteria woke up as babies and went to bed as great-great-great-grandparents. In this way, Lenski and his team have studied more than seventy thousand generations of E. coli over thirty-three years. Compared with their distant ancestors, the latest versions of the bacterium reproduce seventy per cent faster; it once took them an hour to double their ranks, but now they can do it in less than forty minutes. Different populations have taken different paths to enhanced fitness, but, after decades, most have arrived at reproduction rates within a few percentage points of one another.
Lenski’s Long-Term Evolution Experiment, or L.T.E.E., as it’s called, has yielded fundamental insights into the mutational capabilities of microorganisms. For his work, Lenski, now in his sixties and at Michigan State University, has received a MacArthur “genius” grant and a Guggenheim Fellowship. “I’m not sure I can tell you how it’s affected my thinking, because I’m not sure I can conceive of being in this field without this experiment existing,” Michael Baym, an evolutionary biologist at Harvard Medical School, recently told Discover.
Three of the experiment’s key findings are especially relevant today. The first is that, in general, there were diminishing returns to mutation over time: the bacteria made many of their most reproductively advantageous moves early on. A second finding, however, was that the bacteria never stopped getting fitter. Seventy thousand generations in, they’re still finding new ways to improve, albeit at a somewhat slower rate. “I had sort of imagined that things would have flatlined,” Lenski told me recently, when we spoke over Zoom. “But there seem to be endless possibilities for tinkering and progress. If there is a hard limit, it’s so, so far away that it’s impractical to consider on an experimental timescale—maybe even a geological timescale.”
Lenski has a friendly, expressive face, with pale blue eyes and a neat beard; his voice pulses with excitement when he considers a provocative question or explains the implications of his research. He told me about a third major finding: in 2003, some fifteen years and thirty thousand generations into the experiment, Lenski arrived at his lab to find that, overnight, a flask that was normally fairly translucent had turned cloudy. The bacteria it contained had experienced an explosive surge in growth. Normally, E. coli eat mainly glucose, but this population had unlocked an entirely new source of energy: a chemical compound called citrate. The capacity to metabolize citrate is so unusual that no population in the study had developed it until that point, and none have attained it since. It’s as if a family of humans could suddenly drink salt water.
sars-CoV-2, the virus that causes covid-19, has already had one citrate moment: the instant, probably sometime in 2019 but possibly earlier, when it developed the ability to leap into humans. Since then, the virus has accumulated innumerable mutations, some of which allow it to generate copies of itself more efficiently—by altering how it binds to our cells, for instance, or by finding new ways to slip past our immune systems. It’s a process that has occurred with every infectious disease in history—measles, tuberculosis, bubonic plague, influenza, and untold others. The difference with the coronavirus is that the world is now watching every mutational move as it happens.
During this pandemic, we’ve developed and deployed vaccines in real time. Meanwhile, sars-CoV-2 is replicating not in a dozen flasks but in tens of millions of people, some of whom have been immunized, all of whom exert selective pressure for the virus to find new, more efficient replication strategies. The virus will continue to mutate every moment of every day, for years, for decades. The fear is that it will hit upon a second citrate moment: a mutation, or set of mutations, that enables it to circumvent our vaccines, which so far have proved spectacularly effective and resilient. For those who remain unvaccinated—the majority of humankind—there is also the horrifying prospect of a variant that is vastly more contagious or deadly. Every few months, we learn of a version of the virus that seems somehow worse: Alpha, Beta, Gamma, Delta. The coronavirus appears destined to march its way through the Greek alphabet—a prizefighter getting quicker, slicker, stronger with each opponent. What are the limits to its evolutionary fitness? Are they knowable? And, if so, how close are we to reaching them?
These were the questions on my mind as I spoke with experts in an effort to understand the future of the pandemic. With questions so complex, it’s helpful to start by figuring out what, exactly, we want to know. For each new coronavirus variant, we want to find out if it’s more transmissible, if it will make us sicker, and if it will more effectively get around our immune defenses. On that last front, we want to understand two more questions: How much will it succeed in hiding from our antibodies (which recognize and bind to the virus, preventing infection) and from our T cells (which recognize chopped-up viral fragments displayed by infected cells, and specialize not in preventing infection but in controlling and terminating it).
Roberto Burioni, a physician and professor at Vita-Salute San Raffaele University, in Milan, has been called the most famous virologist in Italy; he has written about the prospects for a “final” variant, a version of the coronavirus that has reached maximum transmissibility, and which becomes “the dominant strain, experiencing only occasional, minimal variations.” As Burioni sees it, there are three potential futures for the coronavirus. The first—the most optimistic for us—is one in which the virus simply can’t evolve its way around the vaccines. This is not an unlikely possibility. Many viruses—measles, mumps, rubella, polio, smallpox—have never meaningfully circumvented their vaccines, and so far the best of our current jabs have remained remarkably protective against new coronavirus variants, including Delta….
News
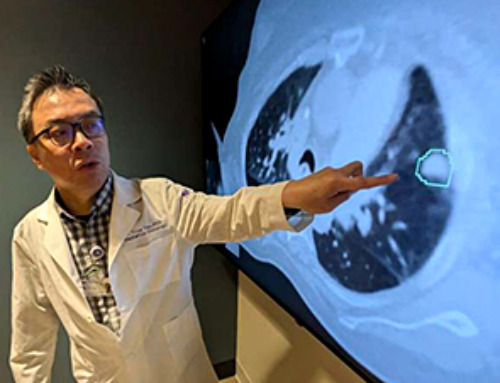
AI matches doctors in mapping lung tumors for radiation therapy
In radiation therapy, precision can save lives. Oncologists must carefully map the size and location of a tumor before delivering high-dose radiation to destroy cancer cells while sparing healthy tissue. But this process, called [...]
Scientists Finally “See” Key Protein That Controls Inflammation
Researchers used advanced microscopy to uncover important protein structures. For the first time, two important protein structures in the human body are being visualized, thanks in part to cutting-edge technology at the University of [...]
AI tool detects 9 types of dementia from a single brain scan
Mayo Clinic researchers have developed a new artificial intelligence (AI) tool that helps clinicians identify brain activity patterns linked to nine types of dementia, including Alzheimer's disease, using a single, widely available scan—a transformative [...]
Is plastic packaging putting more than just food on your plate?
New research reveals that common food packaging and utensils can shed microscopic plastics into our food, prompting urgent calls for stricter testing and updated regulations to protect public health. Beyond microplastics: The analysis intentionally [...]
Aging Spreads Through the Bloodstream
Summary: New research reveals that aging isn’t just a local cellular process—it can spread throughout the body via the bloodstream. A redox-sensitive protein called ReHMGB1, secreted by senescent cells, was found to trigger aging features [...]
AI and nanomedicine find rare biomarkers for prostrate cancer and atherosclerosis
Imagine a stadium packed with 75,000 fans, all wearing green and white jerseys—except one person in a solid green shirt. Finding that person would be tough. That's how hard it is for scientists to [...]
Are Pesticides Breeding the Next Pandemic? Experts Warn of Fungal Superbugs
Fungicides used in agriculture have been linked to an increase in resistance to antifungal drugs in both humans and animals. Fungal infections are on the rise, and two UC Davis infectious disease experts, Dr. George Thompson [...]
Scientists Crack the 500-Million-Year-Old Code That Controls Your Immune System
A collaborative team from Penn Medicine and Penn Engineering has uncovered the mathematical principles behind a 500-million-year-old protein network that determines whether foreign materials are recognized as friend or foe. How does your body [...]
Team discovers how tiny parts of cells stay organized, new insights for blocking cancer growth
A team of international researchers led by scientists at City of Hope provides the most thorough account yet of an elusive target for cancer treatment. Published in Science Advances, the study suggests a complex signaling [...]
Nanomaterials in Ophthalmology: A Review
Eye diseases are becoming more common. In 2020, over 250 million people had mild vision problems, and 295 million experienced moderate to severe ocular conditions. In response, researchers are turning to nanotechnology and nanomaterials—tools that are transforming [...]
Natural Plant Extract Removes up to 90% of Microplastics From Water
Researchers found that natural polymers derived from okra and fenugreek are highly effective at removing microplastics from water. The same sticky substances that make okra slimy and give fenugreek its gel-like texture could help [...]
Instant coffee may damage your eyes, genetic study finds
A new genetic study shows that just one extra cup of instant coffee a day could significantly increase your risk of developing dry AMD, shedding fresh light on how our daily beverage choices may [...]
Nanoneedle patch offers painless alternative to traditional cancer biopsies
A patch containing tens of millions of microscopic nanoneedles could soon replace traditional biopsies, scientists have found. The patch offers a painless and less invasive alternative for millions of patients worldwide who undergo biopsies [...]
Small antibodies provide broad protection against SARS coronaviruses
Scientists have discovered a unique class of small antibodies that are strongly protective against a wide range of SARS coronaviruses, including SARS-CoV-1 and numerous early and recent SARS-CoV-2 variants. The unique antibodies target an [...]
Controlling This One Molecule Could Halt Alzheimer’s in Its Tracks
New research identifies the immune molecule STING as a driver of brain damage in Alzheimer’s. A new approach to Alzheimer’s disease has led to an exciting discovery that could help stop the devastating cognitive decline [...]
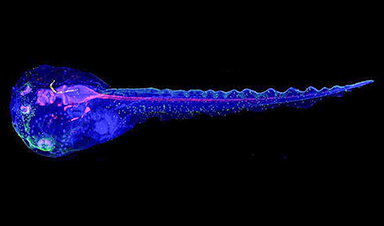
Cyborg tadpoles are helping us learn how brain development starts
How does our brain, which is capable of generating complex thoughts, actions and even self-reflection, grow out of essentially nothing? An experiment in tadpoles, in which an electronic implant was incorporated into a precursor [...]